Fibroids affect an estimated 20 to 50 percent of women of reproductive age, according to UCLA Health. These firm tumors of uterine muscle are almost always benign, but they can develop rapidly under the influence of estrogen and significantly impact the quality of life and fertility of many women.
A variety of treatment options are available, but not many offer fertility preservation and uterine sparing. The ultrasound treatment for fibroids via radiofrequency ablation is one of these very few options. This procedure uses heat to volumetrically ablate fibroid tissue in a controlled thermal zone, which results in coagulation necrosis. Radiofrequency ablation has been used successfully to treat a number of solid abnormalities of the heart, liver and uterine fibroids.
The Radiofrequency Ablation Procedure
Pre-Procedure: Before an ablation can be done, two important things need to be determined: All fibroids must be located and measured, and all contraindications must be excluded. Ultrasound can help with both of these.
Firstly, a transvaginal ultrasound can identify the location and size of all fibroids present, an essential step in ensuring the success of ablation. Secondly, a combination of transabdominal and transvaginal ultrasounds can assist in assessing for contraindications, such as pelvic inflammatory disease, an intrauterine contraceptive device, endometriosis, adenomyosis, gynecological malignancy, cervical myoma, one or more complete intracavitary submucosal fibroids, or significant intra-abdominal adhesions.
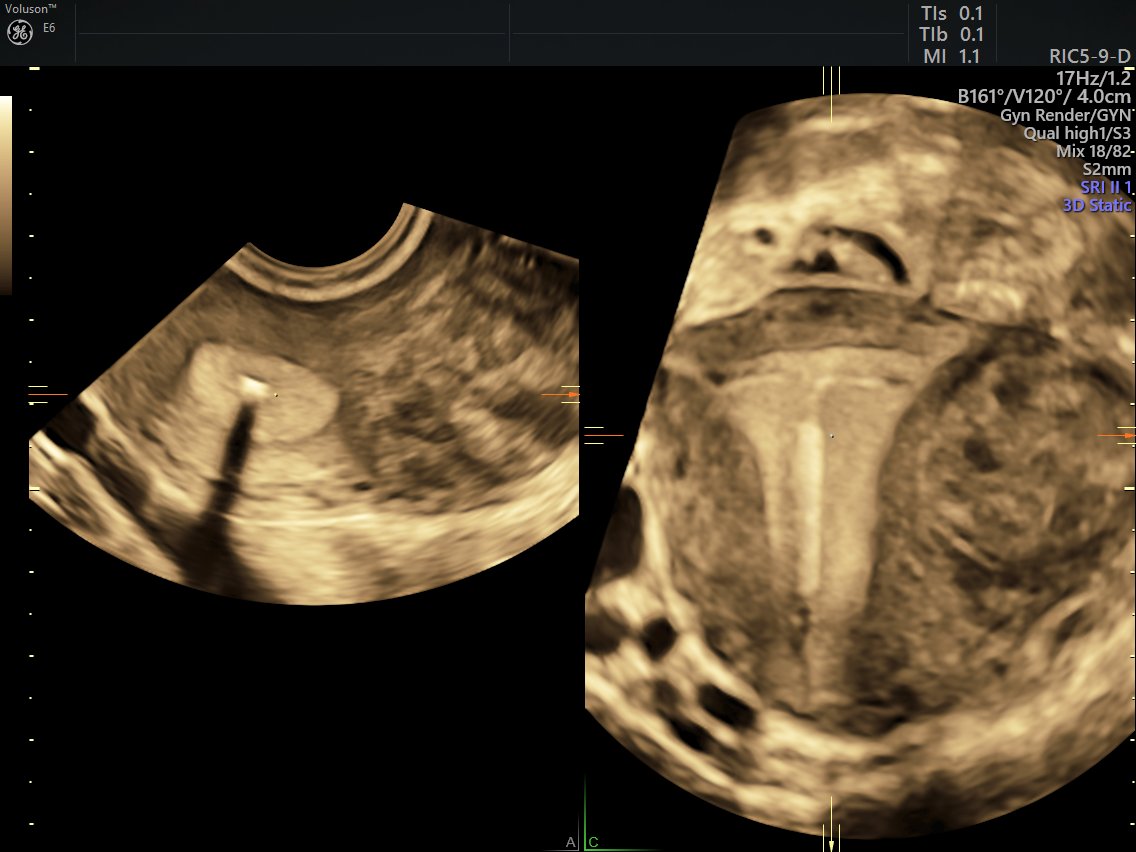
3D image of ultrasound treatment for fibroids
During the Procedure: Each ablation requires the extremely accurate placement of the radiofrequency ablation device. This is to ensure adequate penetration within the fibroid and accurate deployment of needle electrodes while avoiding damage to surrounding normal uterine tissue, blood vessels, nerves and other pelvic structures. A variety of approaches are available for targeting, all of which utilize ultrasound. They include laparoscopic ultrasound, transcervical-intrauterine ultrasound and transvaginal ultrasound.
Post-Procedure: Although radiofrequency ablation of uterine fibroids carries a low risk of complications, each patient must still be carefully monitored after the procedure. Possible concerns include uterine perforation or hemorrhage, hematoma, pelvic abscess, colon laceration and vaginal bleeding. Ultrasound, again, is the modality of choice for this follow-up as it is widely available, non-invasive and accurate.
Why Ultrasound-Guided Radiofrequency Ablation Is So Effective
Fibroid treatments vary widely depending on the type and severity of symptoms, future fertility concerns and whether the patient is a good surgical candidate. Mild symptoms can be treated with medications; however, moderate-to-severe symptoms of pain, bleeding or infertility are most effectively treated surgically.
Hysterectomy is one surgical option that will eliminate all of the fibroids. Myomectomy, the surgical removal of fibroids, spares normal uterine tissue but can lead to extensive myometrial scarring. Recovery is relatively quick and pregnancy is possible after this procedure, but due to concerns about uterine rupture, C-sections are commonly performed.
Uterine artery embolization uses a catheter to cut off blood supply to a fibroid. This reduces the severity of related symptoms without removing the fibroid. While this procedure effectively spares the uterus, the reduced vascularity has been associated with a decrease in ovarian reserve, uterine adhesions and necrosis, along with an increased risk of miscarriage and third-trimester pregnancy complications.
Ablation with radiofrequency and ultrasound treatment for fibroids effectively provides relief from symptoms and improves quality of life as fibroids and overall uterine volume decrease. Treatment of numerous fibroids of varying sizes can be done with one procedure. Radiofrequency ablation uses very small incisions and an insulated shaft to treat fibroids deep within the myometrium without harming the uterine wall. This also avoids damage to the endometrium and uterine blood vessels, which helps avoid limiting future pregnancy outcomes.
The Journal of Minimally Invasive Gynecology reported that fibroid-related symptoms reduce as early as one-month post-procedure, and after one year, the symptoms of pain/pressure, menorrhagia and urinary frequency resolved in 95 to 100 percent of the patients treated.
Radiofrequency Ablation as Minimally Invasive Treatment
The ultrasound-guided treatment for fibroids is proven to be safe, adaptable and efficient in the reduction or elimination of symptoms related to the condition. It can treat fibroids of various sizes and number in a single setting with a rapid and typically uneventful recovery. Patients can return to work often by the fourth day post-procedure, which saves money on healthcare costs.
With a rapid return to work, a low level of re-intervention incidents and a higher rate of normal pregnancies post-procedure, radiofrequency ablation is a positive option when weighing treatments for fibroids.



