Pelvic floor disorders affect millions of women and become more common with age. Pelvic organ prolapse is less common than other pelvic floor problems such as urinary incontinence and fecal incontinence, but still affects nearly 3 percent of women in the United States. In cases of prolapse, 3D and 4D ultrasound provide a cost-saving and convenient first-line option for your patients for identification and diagnosis.
Causes of Pelvic Organ Prolapse
Prolapse happens when the muscles of the pelvis weaken and are no longer able to support the uterus, bladder and rectum, which can press into or protrude from the vagina. Prolapse typically develops later in life, with many women experiencing symptoms at age 60 or older.
Vaginal birth is a common cause of prolapse, as giving birth stretches and strains the pelvic floor muscles and connective tissue. Giving birth to a baby weighing more than 8.5 pounds also increases a person's risk of developing prolapse later in life.
Other causes include:
- Frequent straining during bowel movements
- Chronic coughing
- Obesity
- Menopause
- Genetics
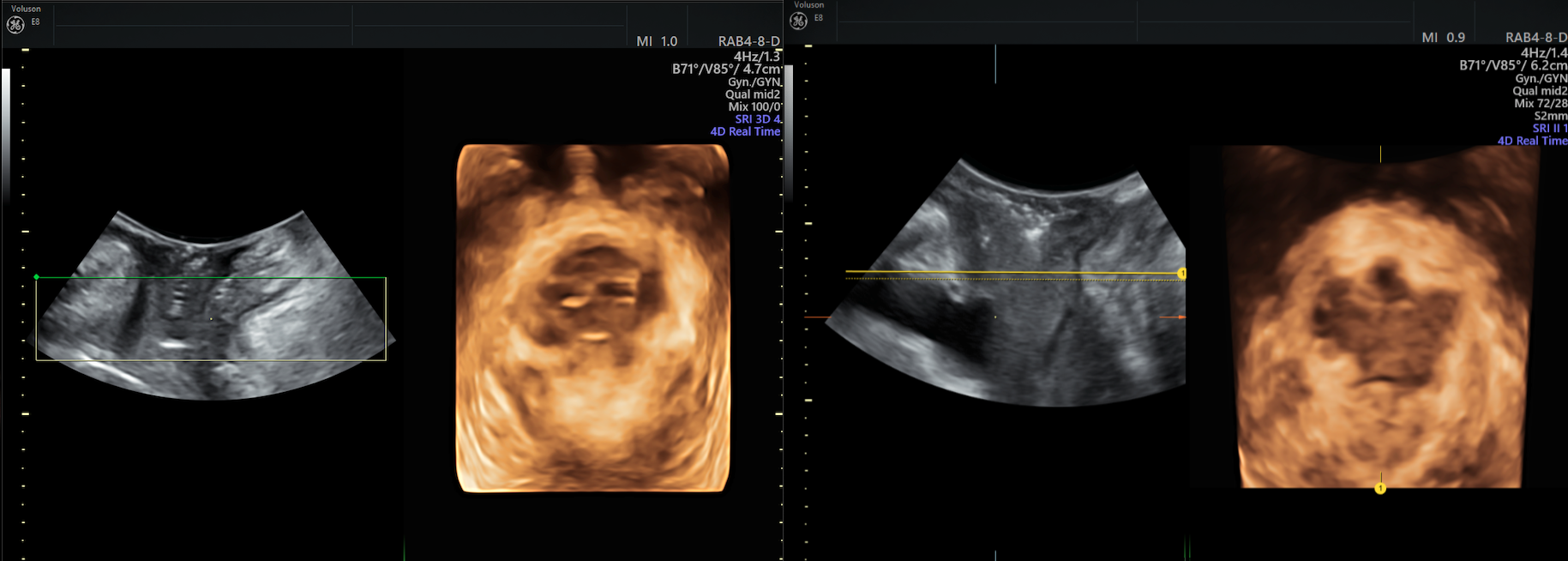
Ultrasound bladder prolapse
Image: Ultrasound of bladder prolapse.
Research has found that women with defects in the levator ani muscle complex have higher rates of prolapse than women without these defects; damage to the levator ani muscles can happen during vaginal childbirth. Women with levator ani defects are also at higher risk of having recurrent prolapse after surgery.
Diagnosing Pelvic Organ Prolapse with Ultrasound
Imaging with 3D or 4D ultrasound allows for accurate evaluation of prolapse with an affordable, accessible tool that many women are already comfortable with. Ultrasound allows you to obtain images of the axial and sagittal planes for a better understanding of the spatial relationships between pelvic organs and connective tissue. Before 3D ultrasound, the axial plane was only viewable through MRI. Ultrasound imaging provides more information for an accurate diagnosis and surgical planning than does MRI or examining the surface anatomy alone.
During the ultrasound exam, have your patient perform the Valsalva maneuver and pelvic floor muscle contractions to allow you to see any pelvic organ descent.
Transrectal, transvaginal and transabdominal ultrasound may be used to assess pelvic floor defects; however, translabial is the most widely used because it is noninvasive. Translabial 3D ultrasound visualizes the axial plane and levator ani, allowing you to look for defects that may require additional monitoring. This technology can also inform which approaches to surgery may be better for patients with severe defects. Avulsion and hiatus ballooning, additional risk factors for recurrent prolapse, can also be seen with 3D/4D volume rendering.
Ultrasound images can help to inform clinicians about the best surgical approach, are beneficial in follow-up and can be used to monitor any mesh or slings that are placed during treatment. Ultrasound is gaining popularity as a second-to-none diagnostic tool for urogynecology because of its affordability and the treatment value of advanced imaging.



