Patients may come into your office with many ideas about endometriosis, but they don't always know the reality of the disease. This can make education, both about endometriosis diagnosis and treatment options, extremely difficult. Let's take a moment now to separate fact from fiction.
Facts from the Medicina:
- Endometriosis is a chronic, debilitating, lifelong inflammatory disease process that affects 5% of the female population.
- Although 40% of women with endometriosis are asymptomatic, the most common signs and symptoms of endometriosis include dysmenorrhea, dyspareunia and chronic pelvic pain.
- Anywhere from 30% to 50% of women diagnosed with endometriosis experience infertility.
Fiction:
- Endometriosis does not occur prior to menarche or in postmenopausal women.
- Pregnancy cures the disease.
- Hysterectomy cures the disease and relieves all symptoms.
Recognizing the Link Between Endometriosis and Infertility
In a patient with endometriosis, tissue containing stroma and glands similar to the endometrium actually thrives outside the uterine cavity. It can occur in the very young and the elderly but is seen more commonly during the reproductive years. Through complex cascades involving cellular and extracellular fluid immunity factors, this tissue grows and causes inflammatory changes.
It can cause pelvic adhesive disease, which disrupts normal anatomy and interrupts normal ovulatory function. It also impedes fertilization and implantation, as these inflammatory chemicals and antibodies hamper ovum, sperm and embryo function. The result is a lowered monthly fecundity and a lower live birth rate.
Evaluating Endometriosis With 3D Ultrasound
When it comes to endometriosis diagnosis and treatment, the goal is early and accurate detection coupled with an individualized management plan to optimize medical therapy and limit multiple surgeries. The first step is a 3D ultrasound of the pelvis, which enables careful examination of the pelvic organs. It is a practical and informative in-office tool for diagnosing a patient with endometriosis.
Ultrasound also allows physicians to map normal and abnormal pelvic anatomy. Adenomyosis, endometriomas, rectovaginal nodules, adherent adnexa, tenderness and tubal patency can be evaluated with a combination of transvaginal 3D ultrasound and saline hysterosalpingography. Tricefy, a cloud-based storage solution, enables clinicians to share the resulting images and consult with colleagues and patients regarding a diagnosis.
Endometriomas, the hallmark of endometriosis involving the ovaries, have a typical ground glass appearance on ultrasound imaging and can range from less than 1 cm to several centimeters in size. Internal wall nodularity, probably representing small clots, should not be mistaken for papillary structures seen with malignancies of the ovaries.
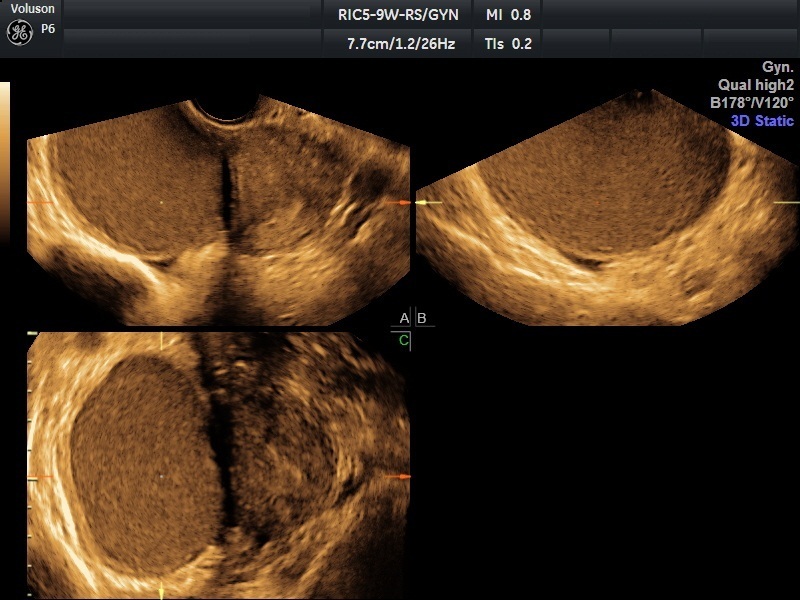
3D ultrasound image of an endometrioma
3D ultrasound is a much-needed safe, non-invasive alternative to laparoscopic surgery for detecting endometriosis in women of reproductive age.

3D Ultrasound with color Doppler
Many endometriosis patients are symptomatic yet undiagnosed for years—or even decades. 3D ultrasound now enables gynecologists to provide answers quickly and painlessly.
Image courtesy of Prof. Stefano Guerriero
Malignant transformation of endometriomas is rare. Atypical endometriomas, including the presence of internal echogenicity, fluid levels and concave-shaped echogenic material consistent with a retracting blood clot, should not be a cause for concern. However, serial ultrasounds may be helpful to document stability or any significant changes.
Creating a Personalized Endometriosis Treatment Plan
If the patient is asymptomatic and not seeking to become pregnant, conservative management of endometriomas is typically the best course of action. If pain or fertility is the issue, careful surgical eradication of all endometriosis and normalization of pelvic anatomy improves both symptoms and fertility.
Preoperative ultrasound can help the surgeon prepare the patient and determine the plan for the surgery. Complete excision of endometriomas, including the pseudocapsule, is recommended, rather than simple drainage and coagulation to reduce recurrence rates. Given that surgery, especially repeat surgeries on the ovaries, may result in reduced ovarian function, documenting whether the endometrioma is uni- or multilocular prior to surgery is important to ensure all endometriomas are removed.
Hormonal medical therapy, including a variety of oral, intramuscular and intrauterine delivery systems, can be used for pain management. However, medical therapy may delay fertility treatment and does not cure the patient. In fact, neither pregnancy nor hysterectomy will cure the patient, seeing as many symptoms can persist. That's why the personalized management plan should always include counseling and patient involvement in the decision-making process.
Finally, if there is a history of treatment failures or other contributing causes for infertility, in vitro fertilization (IVF) and embryo transfer is recommended. If an ultrasound shows that the ovaries are optimally positioned for IVF and the endometriomas do not interfere with access, it may not be necessary to remove the endometriomas. Adhered ovaries or endometriomas that obscure follicles, however, may demand surgical intervention.
Endometriosis is a lifelong debilitating disease that requires an individualized management plan. The age of the patient, the stage of the disease and their symptoms all need to be factored into endometriosis treatment.





