Pelvic pain in women can be acute or chronic in nature. It can occur at any age during a woman's life and always raises concern that something serious, even life-threatening, is occurring. The pain may or may not be gynecology-related, but patients typically visit their gynecologists for initial evaluation and treatment.
The patient may already have a theory as to the cause of the pelvic pain. Listen to her story. Taking a history and physical with appropriate point-of-care testing is still the first step to rule out infections, pregnancy, pelvic masses and other causes of pelvic pain. Your patient's story may tell you if there are contributing factors that need to be addressed. This is an opportunity to share knowledge about normal anatomy and physiology, discuss Mittelschmerz, dysmenorrhea and PMS, and strengthen the patient-physician bond to arrive at a shared decision-making and pelvic pain treatment plan. However, the normalization of pelvic pain has no place in modern medicine.
Using Ultrasound to Examine Causes of Pelvic Pain
One of the most impactful instruments in your pelvic pain tool belt is your point-of-care ultrasound. We know bimanual exams are helpful in diagnosing uterine pathology, but they often miss adnexal problems. Always consider performing an ultrasound for pelvic pain in your office to help lessen your patient's anxiety and reach a diagnosis.
Let's look at three case studies of women with the same chief complaint but very different etiologies for their pelvic pain causes.
Case No. 1
A 27-year-old woman presents with a positive urine pregnancy test three weeks from her last menstrual period, complaining of spotting and pelvic pain. You draw a beta human chorionic gonadotropin (hCG) and conduct a physical exam, which reveals a small amount of blood in the vagina, no active bleeding and mild-to-moderate tenderness in the right adnexa.
Don't wait for the beta hCG level results. An ultrasound will tell you if there is a significant amount of fluid in the pouch of Douglas or whether to rule out ovarian torsion and hemorrhagic ovarian cyst, even if the beta is below the discriminatory level for diagnosis of intrauterine pregnancy. Fortunately for this patient, the only finding is a thick endometrium with the hint of a gestational sac and a corpus luteum cyst on the right ovary. You reassure the patient of their unremarkable pelvic ultrasound, agree to wait for the beta results and schedule a follow-up.
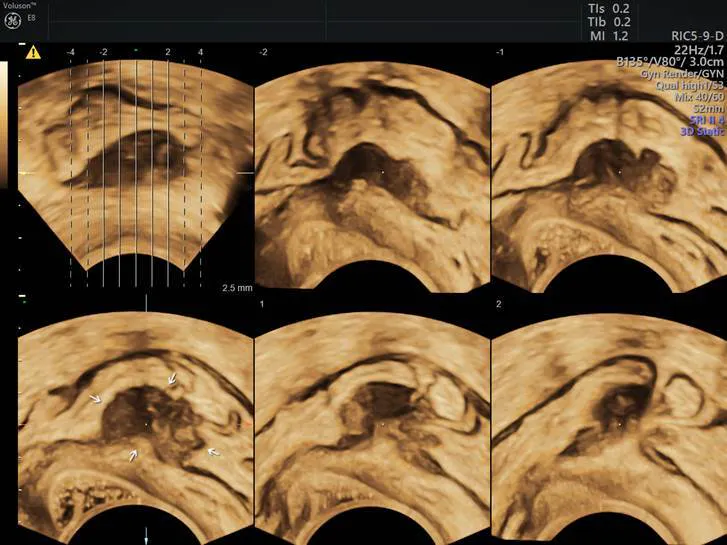
Endo
Deep infiltrating endometriosis with bowel involvement (3D with TUI/tomographic ultrasound imaging).
Case No. 2
A 43-year-old woman presents with painful, heavy periods and a sensation of pelvic pressure throughout the month that has been increasing in severity over the past year. She notes that her mother died of ovarian cancer. Your exam reveals an enlarged uterus that is mildly tender. Her hemoglobin (Hgb) count is nine. The ultrasound helps you map multiple type 1–5 fibroids, and the ovaries appear to be normal. Your review of the results reassures the patient, and you can proceed with developing a plan to manage her symptomatic fibroids and anemia.
Case No. 3
A 61-year-old woman presents with escalating colic-like pain, primarily in the left flank and left lower quadrant. She has a history of infertility due to endometriosis, and a screening colonoscopy one year prior revealed mild diverticulosis. There is no rebound or guarding — bowel sounds are active. The bimanual exam is unremarkable. While the ultrasound confirms the absence of adnexal masses or a thickened bowel wall, a hyperechoic mass with shadowing is noted near the left ureterovesical junction, suggesting a small kidney stone. You discuss findings with the patient and refer her to your urology colleague for management.
Saving Time, Money and Anxiety With 3D Ultrasound
Every woman deserves a careful evaluation each time she presents with pelvic pain symptoms, whether it is the first time or one of many. Although each individual's situation in the above examples is unique, the common thread is pelvic pain. Your expert knowledge of neuroanatomy, causes of pelvic pain in women and point-of-care ultrasound can quickly lead to the development of a treatment plan in many different scenarios. Most importantly, 3D ultrasound can help you manage your patients appropriately and avoid expensive testing or surgical evaluations whenever possible.





