More women than ever are turning to their doctors for access to long-acting, reversible contraception. Intrauterine devices (IUDs) have become a popular solution thanks to their effectiveness and ease of insertion and removal. Currently, two types of IUDs are available for women: the nonhormonal copper IUD (Paragard®) and several hormone-releasing devices (Mirena® and Skyla®).
As a gynecologist, you are in a position to help your patients enjoy greater reproductive freedom through the use of IUDs. An IUD ultrasound can help you evaluate the uterus prior to device placement, implant the device and remove it easily when a patient wishes. Ultrasound is also the preferred method for assessing IUD malpositioning, which may cause a variety of unpleasant symptoms for your patient. Using this technology is an efficient and inexpensive way to help your patients with IUDs stay safe and healthy.
Visualizing IUDs on Ultrasound
2D transvaginal ultrasound has previously been the imaging method of choice for evaluating the uterus prior to IUD implantation and determining IUD placement. However, providers are increasingly turning to 3D transvaginal ultrasound for greater clarity.
Copper IUDs appear differently on ultrasound than levonorgestrel-releasing IUDs. The device features a T-frame made of polyethylene, with copper wire coiled around the stem and both horizontal crossbars. The copper enhances sonographic visualization and can be readily seen via 2D ultrasound in both the sagittal and transverse planes. Ring-down artifacts are common in 2D images of copper IUDs.
In contrast, hormone-releasing IUDs feature a polyethylene T-frame, which includes a small hormone-containing reservoir on the stem. Given that there is no metal present in this device, 2D imaging is not as effective for an IUD in uterus ultrasound.
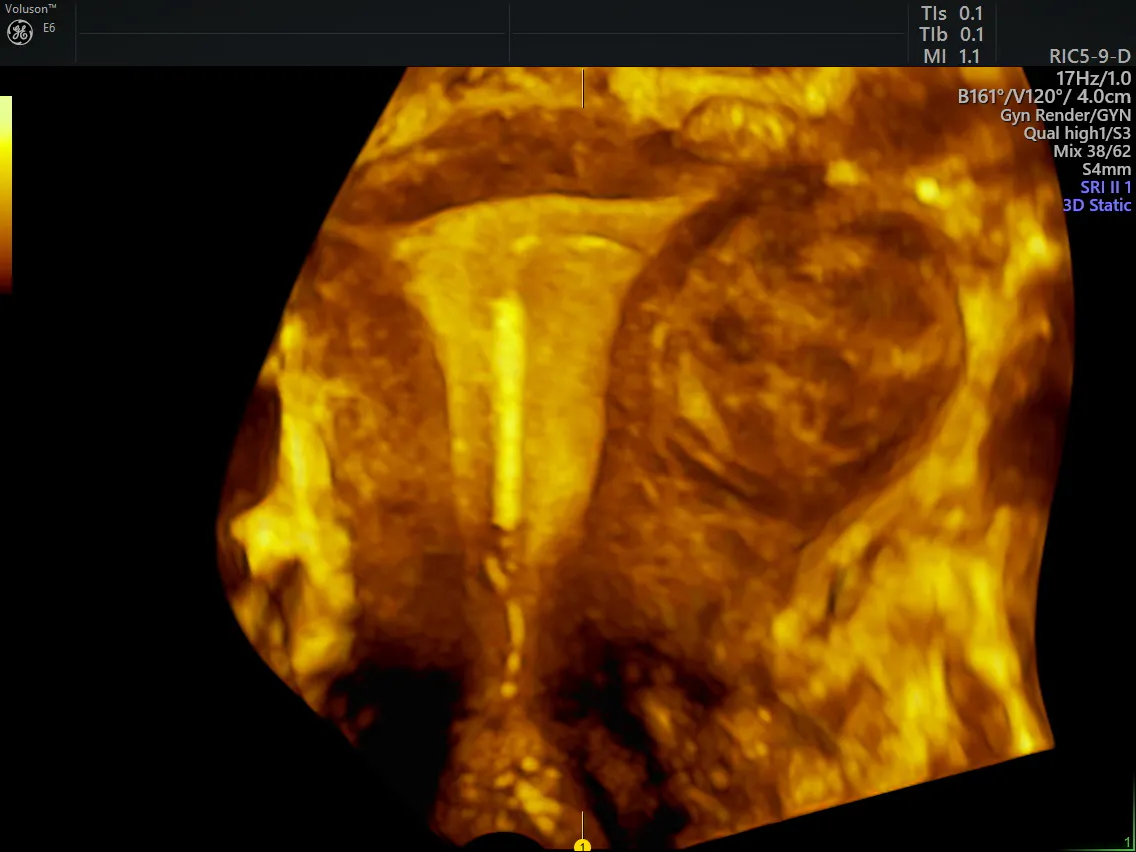
copper IUD ultrasound in 3D
2D vs. 3D: IUD Placement Ultrasound
A study published in the American Journal of Roentgenology found that even though copper IUDs could be readily visualized on 2D transvaginal ultrasound, hormone-releasing IUDs were not as easy to identify. In many cases, only portions of the hormonal IUD shaft were visible, along with a shadow of the intersection of the stem and IUD arms. The study did note that the acoustic shadow of the device could be used to identify it, but that this technique is not a reliable method for determining the implant's precise location.
3D imaging improves the conspicuity of each type of IUD. 3D ultrasound, which offers the benefit of visualization in the coronal plane, allows you to better determine proper positioning of the IUD within the uterine cavity. Because you can obtain a volume rendering with 3D ultrasound, you can also see the entire device within the endometrial cavity. Determining the precise placement of either type of IUD is much simpler using this type of imaging.
Using 3D Ultrasound for Improved IUD Placement
3D ultrasound offers additional benefits to providers and patients alike. Some women with IUDs experience symptoms such as dysmenorrhea or heavy bleeding. In such cases, you can easily locate a malpositioned device using IUD ultrasound. According to research published in Contemporary OB/GYN, 3D ultrasound correctly identifies 84 percent of incorrectly placed IUDs, compared to 65 percent using 2D ultrasound.
To avoid malpositioning problems, consider using 3D ultrasound to verify an IUD's placement after insertion into the uterus. If necessary, 3D imaging can also be used to help remove malpositioned IUDs.
While 2D transvaginal ultrasound can provide valuable information about certain types of IUDs, 3D ultrasound offers greater visualization for all types of implantable devices. This technology, which you can use right in your office, offers a fast, convenient and cost-effective method of assessing both your patient's individual anatomy and their IUD placement.
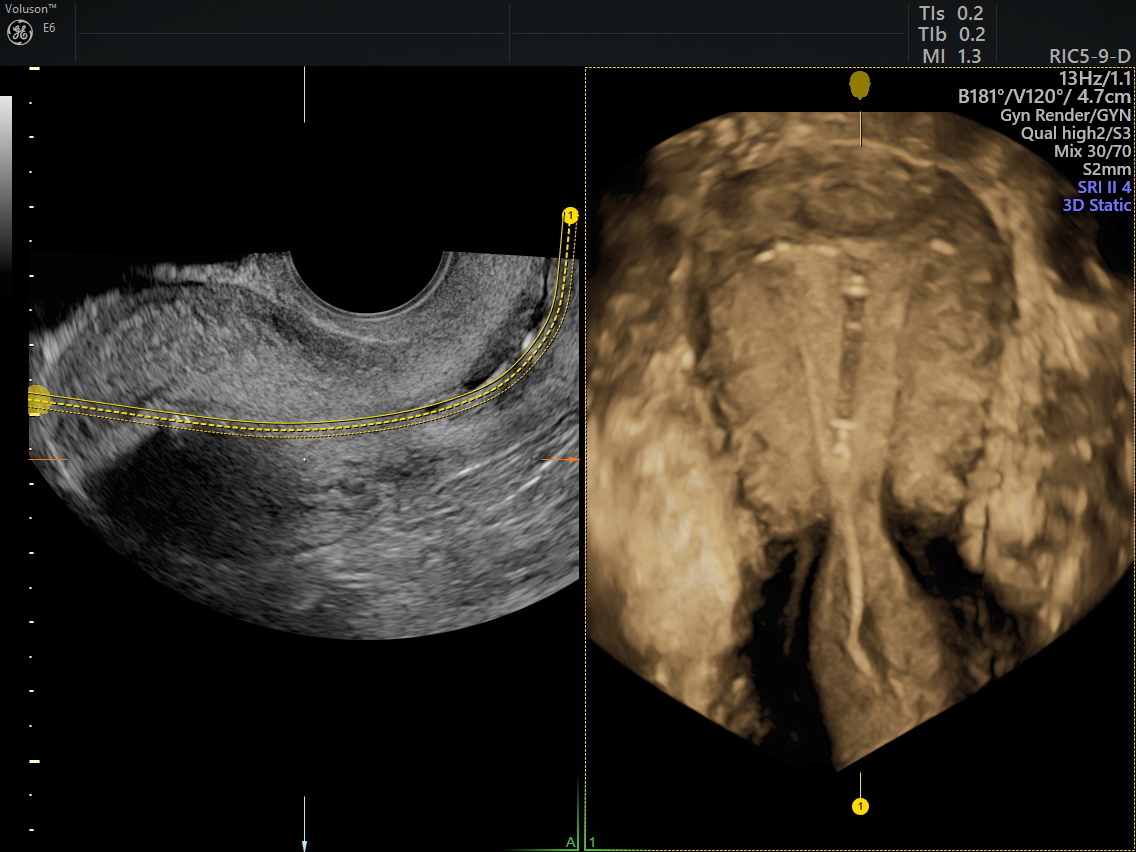
Mirena IUD ultrasound image in 3D