
IUD Insertion with Ultrasound Guidance
Ultrasound Can Simplify the Procedure and Minimize Risk

Discover how Ultrasound can simplify the procedure and minimize misplacement when inserting an IUD.

With more than 168 million users, the intrauterine contraceptive device is the most popular reversible form of contraception around the world.1 IUDs are more than 99% effective, but they require proper placement to provide the best protection.
It doesn’t matter if she’s just dating, or her kids are already done with diapers. Every woman wants to know that her contraception works. With an IUD, your patient is relying on you for accurate and precise placement.
“It’s not a difficult procedure, but it’s a blind procedure for many clinicians,” said Lisbet Hanson, M.D., of Medical Director of Sentaras Women’s Health Program at Virginia Beach General Hospital. “If you don’t do an ultrasound to see if the IUD is in the correct position, you don’t really know for sure.”
While there are no specific guidelines that say scanning is necessary for IUD insertion, transvaginal 3D ultrasound can simplify the procedure and minimize risk. Even the most experienced physicians can encounter complications during the insertion process—including expulsion, displacement, embedment and perforation. In fact, research shows uterine perforation occurs about once in every 1,000 insertions.2
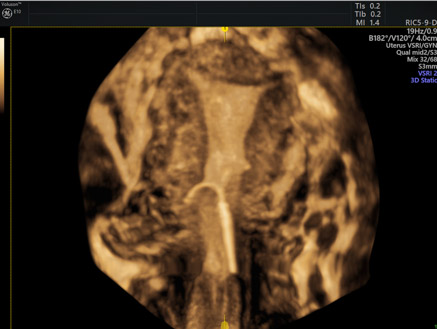
3D images of misplaced IUD
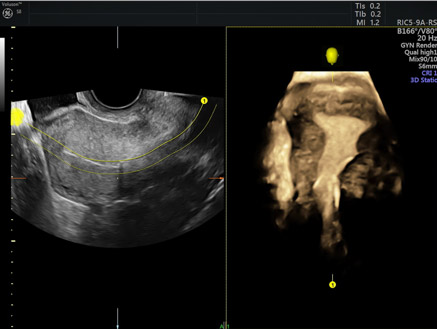
3D images of misplaced IUD
Bernard Benoit, M.D. of Princess Grace Hospital in Monaco insists on performing an ultrasound before every IUD procedure. He relies on 3D ultrasound for his initial assessment because it provides views that aren’t possible with 2D imaging.
“With 3D, you can move to that coronal plane view and see if there are any contraindications. You can see the exact shape of the uterine cavity. You can also measure the volume and the length of the uterine cavity,” Benoit explained.
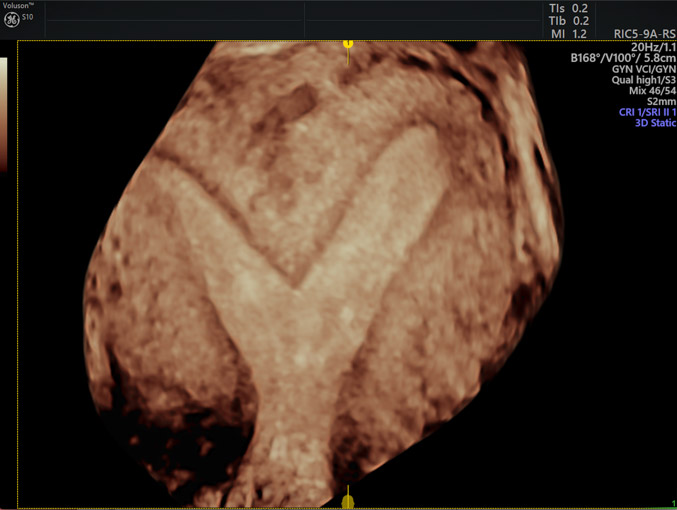
Subseptate uterus (3D)
This information is especially important when you consider research that shows most conventional IUDs are too big to fit inside the uterine cavities of many women.2-5
“I’ve seen a lot of IUDs in the wrong position and many times the uterine cavity was just too small,” Benoit said. “With 3D ultrasound, I can also see if the cavity is too big or if there is a deformity—and that can affect which intrauterine device I choose.”
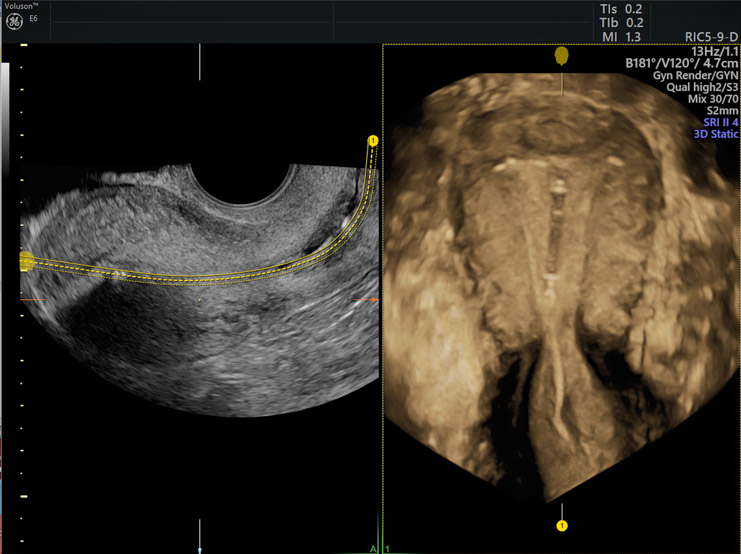
Mirena® IUD (3D)
Both Dr. Benoit and Dr. Hanson depend on VolusonTM ultrasound technology from GE Healthcare to be their guide. The high-resolution images show the endometrium in extraordinary detail. 3D imaging with OmniView allows for greater confidence in evaluating the entire uterine cavity for the best possible outcomes. The advanced ultrasound tools can also empower patients.
“There are a lot of women who think their IUD isn’t doing anything because they can’t see it or feel it—and that makes them worry,” Hanson noted. “I like to show my patients the detailed ultrasound images so they can see their IUD is in the right place, and that makes them feel a lot more confident about their birth control.”
-
When no identifiable IUD strings are located, IUD removal can be completed successfully in the office with a few simple instruments under ultrasound guidance.
-
What is ultrasound used for? Ultrasound has many applications for women's health, far beyond just obstetrics. Read our collection of FAQs.
-
For women who are nearing menopause but still experiencing monthly periods, intrauterine devices (IUDs) are a good choice for contraception.
-
Providers should follow the latest AIUM ultrasound guidelines to ensure they're equipped to provide high-quality, up-to-date care to their patients.
-
By catering to the concerns of women of fertility age, gynecologists can develop strong relationships that can last well past menopause.
-
Reproductive aging in women has an ovarian and uterine component. Doctors should use ultrasound and blood tests to assess ovarian reserve and oocyte health.
-
When trying to identify symptoms of infertility in women, transvaginal ultrasound should be the first test gynecologists recommend in diagnosing infertility.
-
Try out this fun exercise and learn more about the benefits of ultrasound in GYN diagnosis.
Teal SB, Sheeder J (2012) IUD use in adolescent mothers: retention, failure and reasons for discontinuation. Contraception 85: 270–274.
Rasheed SM, Abdelmonem AM (2011) Complications among adolescents using copper intrauterine contraceptive devices. Int J Gynaecol Obstet 115: 269–272.
Kaislasuo J, Suhonen S, Gissler M, Lähteenmäki P, Heikinheimo O (2013) Uterine perforation caused by intrauterine devices: clinical course and treatment. Hum Reprod 28: 1546-1551.
Shipp TD, Bromley B, Benacerraf BR (2010) The width of the uterine cavity is narrower in patients with an embedded intrauterine device (IUD) compared to a normally positioned IUD. J Ultrasound 2010 Dec;29(12):1848.


