When a patient embarks on an assisted reproductive journey, one of the first steps is ultrasound-guided oocyte retrieval. Making this procedure more effective helps to improve the patient's overall experience and can increase their chances for a relaxed and healthy pregnancy.
Transvaginal ultrasound-guided oocyte retrieval, which first began to replace laparoscopic retrieval in 1985, has become essential to modern assisted reproductive technology. The oocyte or egg retrieval procedure is considered safe and effective, but it can be quite painful for patients. The pain is mainly caused by puncture of the vaginal wall and ovarian capsule as well as by necessary manipulation of the ovaries. Advances in ultrasound technology and the tools used in tandem with it — such as a new needle design — may help reduce pain for patients undergoing this procedure.
A Less Painful Procedure With Ultrasound
Compared with older laparoscopic methods, ultrasound makes oocyte retrieval faster, less invasive and more straightforward for surgeons. Transvaginal ultrasound also allows doctors to use a wider variety of pain relief methods for patients undergoing a retrieval procedure.
For many years, conscious sedation has been the standard for preventing pain while retrieving oocytes. The Journal of Human Reproductive Sciences showed patient acceptance and satisfaction rates for this method of anesthesia were high: 86 percent of patients preferred conscious sedation for future procedures after they had experienced it.
Ultrasound Improvements: From 2D to 3D
Recent improvements in ultrasound technology are helping providers visualize the retrieval procedure better than ever before. According to Reproductive Biomedicine Online, newer 3D ultrasound imaging has allowed more oocytes to be retrieved overall when compared with 2D ultrasound. Additionally, more oocytes retrieved with this technology were ultimately fertilized on the first day.
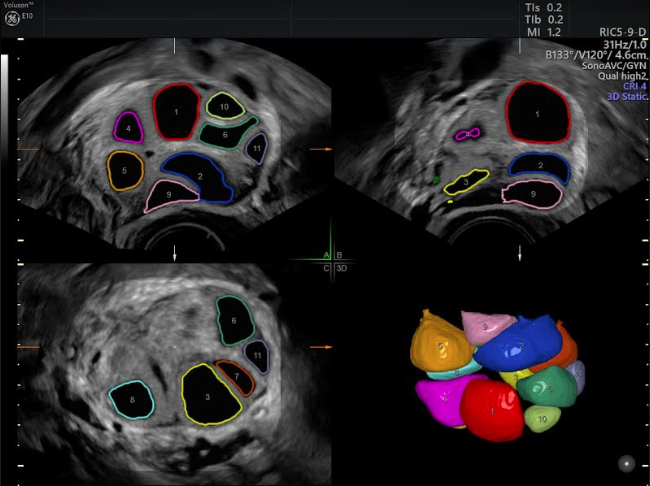
[Automated Follicle Count with SonoAVCfollicle]
During the retrieval procedure itself, 3D ultrasound also allowed follicles to be measured faster and more consistently among surgeons. Because in vitro fertilization (IVF) success is highly dependent on follicle size — a measurement of 12–19 millimeters is most likely to yield a mature oocyte — getting this information more quickly may put patients at ease and aid fertility plan discussions.
Using Thinner Needles
The protocol for ovarian stimulation has changed from hyperstimulation to minimal stimulation, meaning the dosage of fertility drugs administered is reduced. This has helped to increase the safety and efficiency of the retrieval procedure.
However, it can be painful when even a single follicle is punctured. Traditionally, a 19-gauge needle has been used; but smaller needles, such as those with a 20-gauge tip, have been associated with less post-procedural pain and bleeding. The use of thinner needles does not prolong the retrieval procedure and has shown no negative results on oocyte retrieval rate or fertilization chances.
Using a thinner needle does come with some risks: It can make it more difficult to visualize the needle while retrieving the target follicle. Taking this concern into consideration, Vitrolife developed the Sense needle, which features only a thinner 20-gauge needle tip and a 17-gauge needle body. Each movement of the needle is visualized via ultrasound during the procedure—every millimeter is critical for accuracy and patient comfort.
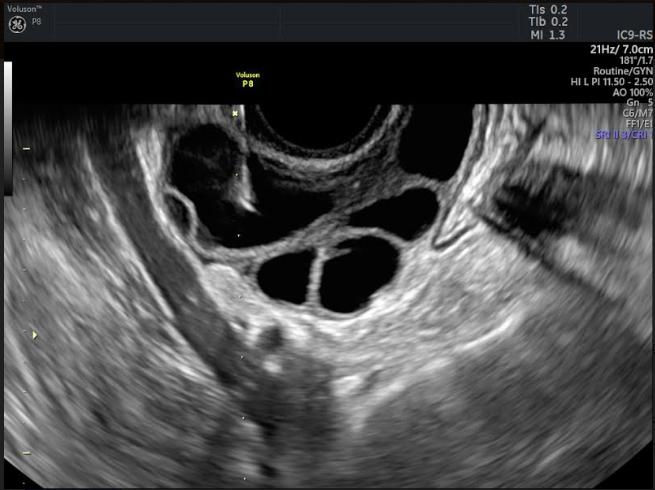
[Oocyte Retrieval With Sense Needle]
The Future of Ultrasound-Guided Oocyte Retrieval
Research continues to improve egg retrieval for patients and providers. Coupled with new needle technology, ultrasound-guided oocyte retrieval ensures pickup at the optimal time and an overall decrease in patient discomfort. These improvements offer more effective tools for providers and less anxiety for patients.





