Polycystic ovarian syndrome (PCOS), also known as hyperandrogenic anovulation or Stein–Leventhal syndrome, is a multifaceted collection of signs and symptoms. Since this condition is a complex syndrome, no gold standard criteria exist for a quick and easy PCOS diagnosis.
However, the National Institutes of Health and the Rotterdam Criteria agree on three main guidelines for the diagnosis of PCOS: menstrual irregularity, hyperandrogenism and polycystic ovaries on ultrasound. This last symptom commonly presents as an ultrasound marker known as the string of pearls.
Ultrasound Features for PCOS Diagnosis
When PCOS is suspected and a pelvic ultrasound is necessary to evaluate the appearance of the ovaries, it's helpful to know how to identify the specific ultrasound features of PCOS. Only one ovary has to be polycystic to raise any suspicions.
A polycystic ovary must have at least one of the following:
- Presence of 12 or more ovarian follicles (measuring 2–9 mm), arranged peripherally in the ovary like a string of pearls.
- Increased ovarian volume to greater than 10 cm.3
- Hyperechoic stroma.
The most obvious ultrasound sign will be the first one, where the follicles of the ovary are more prominent than normal and appear in a row along the edge of the ovarian tissue. Follicles can also multiply to the point of appearing like a cluster of grapes (the other nickname for PCOS's appearance on ultrasound) within the ovarian stroma. It is these enlarged follicles that increase the volume of the ovary to more than 10 cm3.
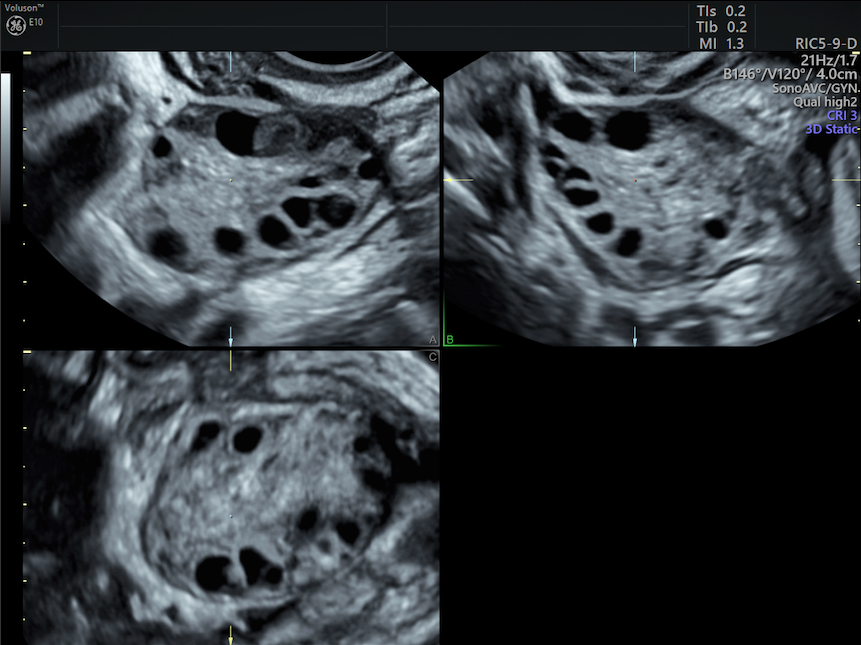
polycystic ovaries on ultrasound
Best Practices for Visualizing a Polycystic Ovary on Ultrasound
3D transvaginal ultrasound provides the most detailed view of ovarian tissue. If 3D ultrasound is not available, using 2D transvaginal ultrasound with a cine sweep through both the sagittal and transverse planes of each ovary can provide adequate information on ovarian size and number of follicles. In situations where transvaginal ultrasound is contraindicated (as with non-sexually-active or young patients), transabdominal ultrasound can be used instead.
It is imperative to ensure that the patient's bladder is not overly full when doing a transabdominal assessment of the ovaries. A half- or one-third-full bladder is preferable in most patients to minimize the compression of the ovary and give the most accurate measurements.
Document any strings or clusters of follicles and clearly label the number of follicles in each ovary to determine whether the minimum number and size requirements are met. When calculating the volume of the ovaries, measurements in three dimensions (anteroposterior, transverse and width) are required for both the ovaries beginning in the longest plane of the ovary.
A careful comparison of ovarian stroma to surrounding tissue may be necessary to determine if increased echogenicity is present. A split-screen image can also be helpful to compare bilateral ovaries.
The Complexity of the Polycystic Ovary
One caveat clinicians must be aware of is that polycystic ovaries are a surprisingly common finding in healthy patients who do not have PCOS. For this reason, a study published in Human Reproduction argues that the threshold for determining a polycystic ovary should be increased from 12 follicles to 26. Research published in the journal Gynecological Endocrinology found that more than 83 percent of healthy women ages 18 to 22 have at least one polycystic ovary. This prevalence of polycystic ovaries in the general population appears to decrease with age.
Keeping this in mind, the educated clinician will know that not every string of pearls glimpsed on ultrasound will lead to a PCOS diagnosis. However, ultrasound exams can be a critical factor in the search for answers for patients with PCOS.





