The American Congress of Obstetricians and Gynecologists (ACOG)-recommended annual Well-Woman exam focuses on providing preventative care through the routine assessment of breasts, reproductive organs, sexually transmitted infections, family health risk factors and overall health history.
Although this annual exam utilizes many modern tests such as electrocardiography and blood work, it still relies on the relatively archaic bimanual pelvic exam to assess the cervix, uterus and ovaries. A more sophisticated method, widely available but not yet widely utilized in routine annual checks, is to conduct a pelvic or gynecological ultrasound, which delivers an incredible improvement in the detail of the reproductive organs.
There are a number of ways in which a pelvic ultrasound can improve a clinician's ability to accurately diagnose gynecological concerns. Let's examine the main areas of the pelvis and their dominant concerns.
The Cervix
While a Pap smear is an excellent method for assessing the presence of cancerous cervical cells, there are many other pathologies by which the cervix can be affected. When cervical motion tenderness is noted during an exam, it can raise a flag for pelvic inflammatory disease (PID), which can be difficult to diagnose due to its subtle symptoms but comes with serious complications such as tubo-ovarian abscesses and ectopic pregnancy. Fortunately, both of these can reliably be ruled out with a transvaginal ultrasound.
Cervical polyps, while benign, can be the cause of spotting, heavy periods, bleeding after intercourse and even infection. They are easily treated, but to remove them a physician must first identify them. Polyps are often so small that they can only be seen with a transvaginal ultrasound.
The Uterus
Palpating a bulky uterus during a bimanual exam can lead to questions about the presence of fibroids, adenomyosis or even a bicornuate uterus. Fibroids and adenomyosis can be the cause of heavy, painful menstrual periods, pain during intercourse and continual pressure in the lower abdomen. A bicornuate uterus can cause miscarriages or difficulty carrying a pregnancy to term.
With a gynecological ultrasound, particularly a transvaginal one that utilizes 3D technology, physical signs of uterine disorders are easily imaged and assessed to provide immediate feedback to patients, allowing for a treatment plan to begin that day.
The Adnexa
When palpating the pelvic adnexa in search of the ovaries, the detection of a possible mass could mean the presence of an ovarian or paraovarian cyst, endometrioma, dermoid cyst/teratoma or ovarian cancer.
Many ovarian cysts are painful and can come with the risk of ovarian torsion. But the most concerning ovarian cysts are in postmenopausal women. These can be cancerous and are often found too late to prevent metastasis.
Having access to an immediate pelvic ultrasound, particularly a vaginal ultrasound, allows clinicians to quickly differentiate between suspicious and benign cysts or masses on or around the ovaries. Point-of-care ultrasound produces immediate results and eliminates the need for patients to wait for an additional appointment.
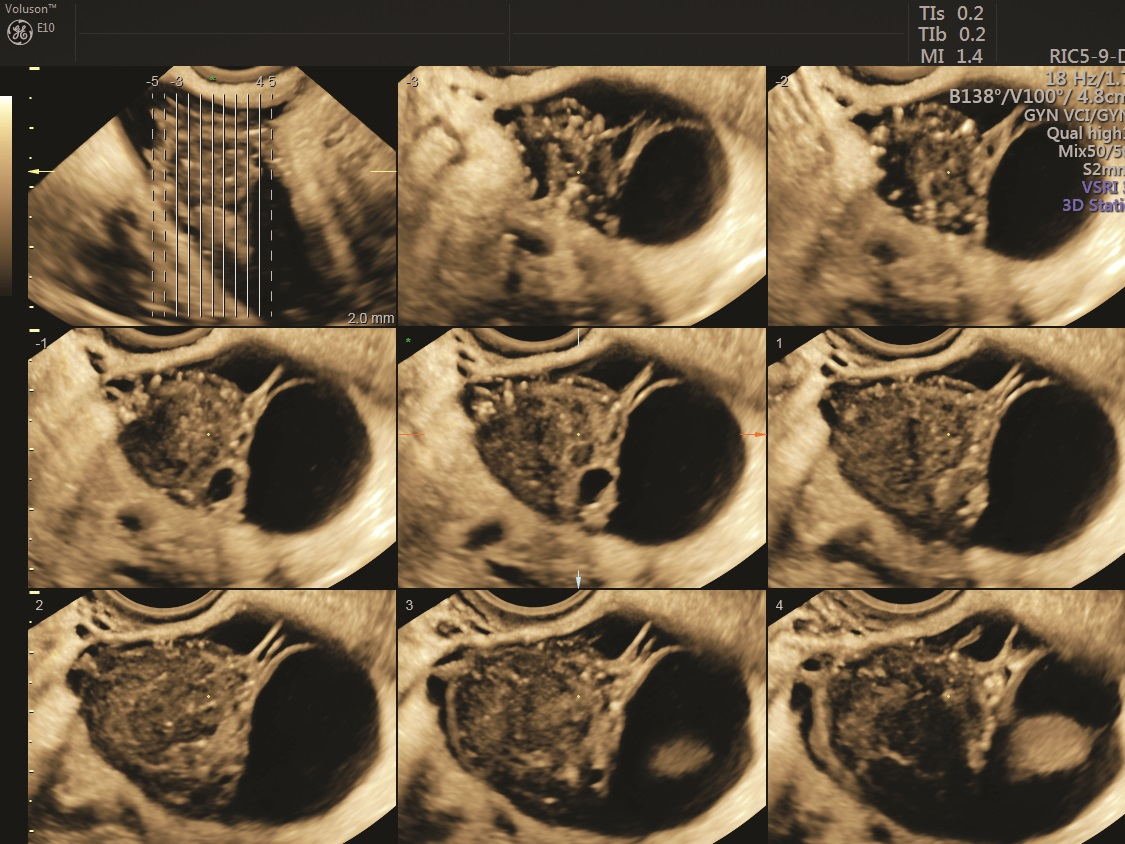
TUI gynecological ultrasound image
Building a Modern Practice
It may be time to accept that the bimanual pelvic exam is no longer the most effective or efficient tool for assessing the female pelvis. Ultrasound is rapidly proving to be a better method of assessment that reliably offers the necessary details and clarity of the reproductive organs with same-day results.
Modern assessment tools provide clear benefits for both clinicians and patients. The wave of the future is to be able to remove the guesswork and the need to book future appointments, whether a patient has a history of abnormalities, symptoms of irregularity or concerns about family history and just wants peace of mind.



