Polycystic ovary syndrome (PCOS) is the most common endocrine abnormality affecting women of reproductive age, but this condition is still not completely understood. Patients with PCOS can experience a wide range of symptoms and health concerns, including infertility, metabolic problems, obesity, hyperandrogenism and abnormal menstrual cycles.
In an attempt to provide unified PCOS diagnostic criteria, a panel of experts from the American Society for Reproductive Medicine (ASRM) and the European Society for Human Reproduction and Embryology (ESHRE) met in Rotterdam in 2003 for a consensus workshop. They devised what would become the Rotterdam criteria for PCOS ultrasound and physical markers alike.
The criteria are widely used to diagnose the condition, but they are based on expert opinion, not evidence-based treatment guidance. So how relevant are these diagnostic guidelines today?
What Are the Rotterdam Criteria?
Because PCOS can be complex — and does not always involve polycystic ovaries — the 2003 consensus sought to develop a standardized basis for diagnosing the condition and beginning treatment. Past clinical recommendations for PCOS had been spotty and contradictory; earlier diagnostic criteria from the National Institutes of Health in 1990 did not even list polycystic ovaries as a symptom.
According to the Rotterdam criteria, a clinical diagnosis of PCOS requires that a patient present with two of the following symptoms:
- Oligo-ovulation or anovulation.
- Hyperandrogenism, clinical (including signs such as hirsutism) or biological (including a raised free androgen index or free testosterone).
- Polycystic ovaries visible on ultrasound.
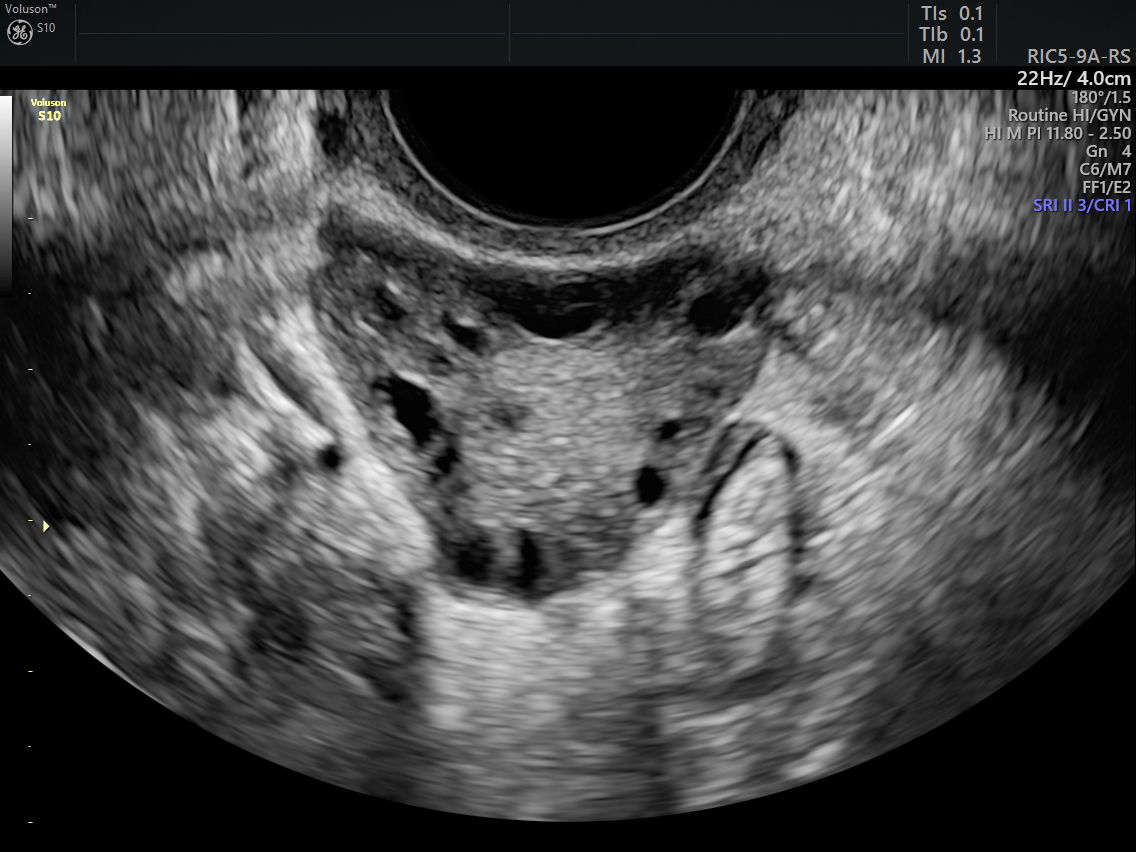
Transvaginal ultrasound of polycystic ovary
The addition of ultrasound assessment of ovarian cysts was a key improvement upon past diagnostic measures. Transvaginal ultrasound provides better visualization for evaluating polycystic ovaries than transabdominal ultrasound.
With the establishment of the Rotterdam criteria, the prevalence of PCOS expanded, possibly by as much as 50 percent, according to a study published in BJOG. However, polycystic ovaries are not an uncommon ultrasound finding, which is why at least one other condition must be met for a PCOS diagnosis, and why clinicians must work to exclude other possible causes.
Are the Criteria Still Relevant?
These criteria have been used to guide research and predict reproductive prognosis, but there is some debate as to whether this consensus opinion guides treatment effectively. PCOS is a complex condition to diagnose and treat because of how varied its presentation can be. An individual patient's situation can also be complicated by linked conditions such as hypothyroidism and insulin resistance or diabetes.
Research published in Human Reproduction sought to evaluate whether the criteria can go beyond research and diagnostic purposes to guide treatment for infertile patients. The authors felt that the World Health Organization's classification of anovulation was a more effective avenue for guiding treatment in patients with oligo-anovulatory infertility and PCOS. The researchers also found that while the criteria were useful in predicting reproductive outcomes, they were not comprehensive, meaning that additional factors should also be considered when determining a PCOS prognosis.
Although there's some controversy surrounding these criteria, many reproductive societies and clinicians still recommend their use. In 2006, the Androgen Excess Society released a position statement in the Journal of Clinical Endocrinology and Metabolism that accepted much of the criteria but expressed a preference to define PCOS first as a disorder of androgen excess or hyperandrogenism.
The position statement supported a diagnosis based on two of the three symptoms laid out in the Rotterdam criteria but added a fourth bullet point to exclude other potential disorders that can mimic PCOS, including Cushing's syndrome and thyroid dysfunction. The Endocrine Society published similar recommendations for using the criteria to diagnose PCOS in American Family Physician in 2016.
Until they are replaced by evidence-based treatment guidelines, the Rotterdam criteria remain the recommended avenue for forming a PCOS diagnosis. However, additional research on any comorbidities and specific symptoms should be considered in determining the best PCOS treatment for an individual patient.





