According to the Centers for Disease Control and Prevention, approximately 6.1 million — roughly 10 percent of women ages 15-44 in the U.S. — experience infertility, or difficulty achieving or keeping a pregnancy. A full evaluation to determine the root cause can be costly and take several months to complete, since both partners need to be examined. A simple semen analysis is the primary way to check for male factor infertility, but what is the first step for women who may be experiencing infertility symptoms?
Sometimes, women who are not actively seeking pregnancy request fertility testing to help them determine whether there is cause for concern if they postpone pregnancy. Reassurance alone may be soothing, but many want concrete evidence that there is no major problem that could interfere with future fertility.
Physicians need a simple, noninvasive tool that delivers the information necessary to determine whether the patient requires a deeper dive into testing. I would argue that a transvaginal ultrasound infertility test should be the first place you start.
The Pros and Cons of the Fertility MOT
The fertility MOT, a quick test to assess fertility, is a hot topic of discussion. M stands for the man: A semen analysis evaluates the sperm count, morphology and motility. O stands for ovulation and ovarian reserve. T stands for ana-T-omy — structural problems that may prevent pregnancy or result in recurrent pregnancy loss.
The test includes a limited number of exams for both the man and woman who may be unknowingly experiencing infertility symptoms. Of course, there are deficiencies. For example, the fertility MOT does not assess the quality of an egg, and it cannot guarantee a healthy newborn in the future. In addition, since the single most important factor impacting fertility is a woman's age, there is a date of expiration for the test results.
A study published in the Journal of the American Medical Association challenged the notion that the biomarkers of ovarian reserve in the fertility MOT can provide an estimate of fertility potential. The authors concluded that in women ages 30–44, abnormal biomarker results do not necessarily correlate with infertility. Still, screening fertility tests can help appease fears and allow women to plan their education, career and family. As clinicians, it behooves us to respond to our patients' fears with compassion and understanding as well as information about the limits and benefits of testing.
Using Ultrasound To Screen for Infertility Symptoms and Signs
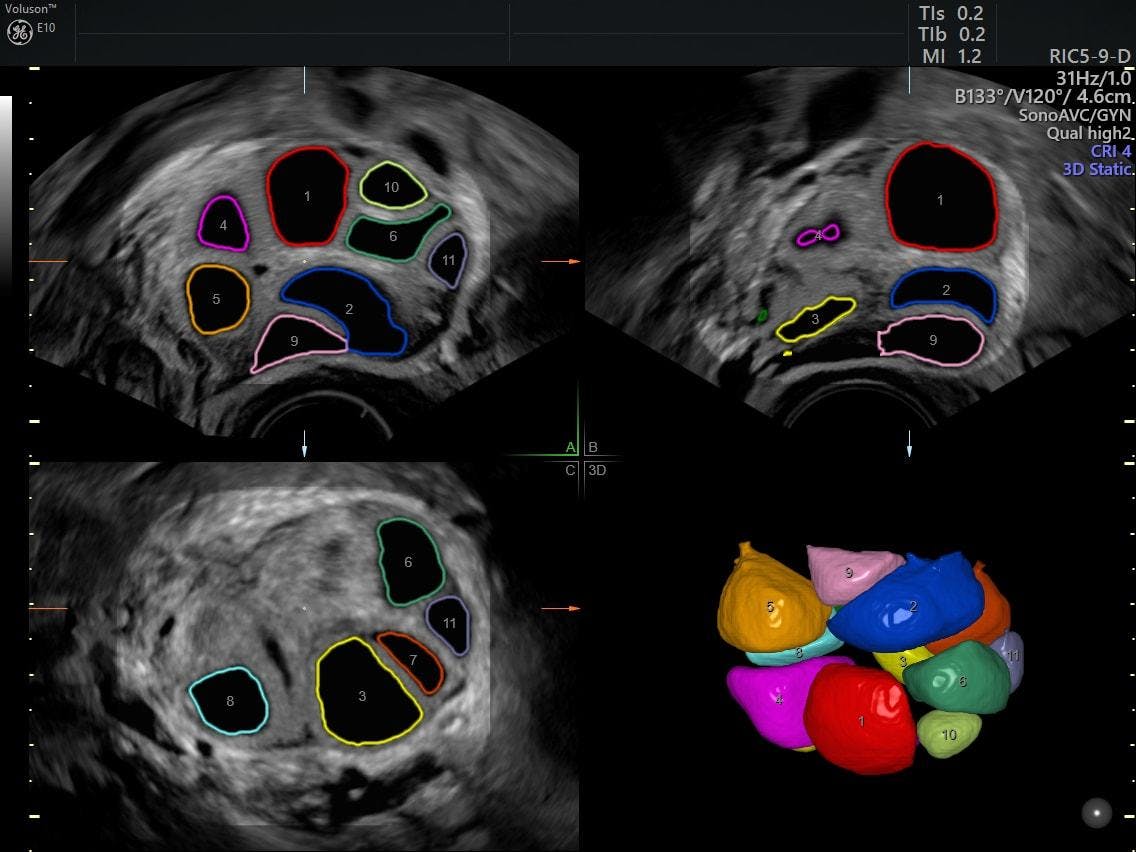
Both a lab test for anti-Müllerian hormone (AMH) and a pelvic ultrasound can provide insight into ovarian function. AMH, a glycoprotein produced by the primordial follicle, is used in patients undergoing in vitro fertilization (IVF) as a marker for ovarian reserve. A high AMH value has been associated with higher conception rates, while low values have indicated a poor ovarian reserve and conception rate. Another marker for ovarian reserve is the antral follicle count, an ultrasound evaluation of egg supply. This can be performed as a 2D real-time ultrasound to check fertility or using stored 2D cineloop and stored 3D ultrasound images.
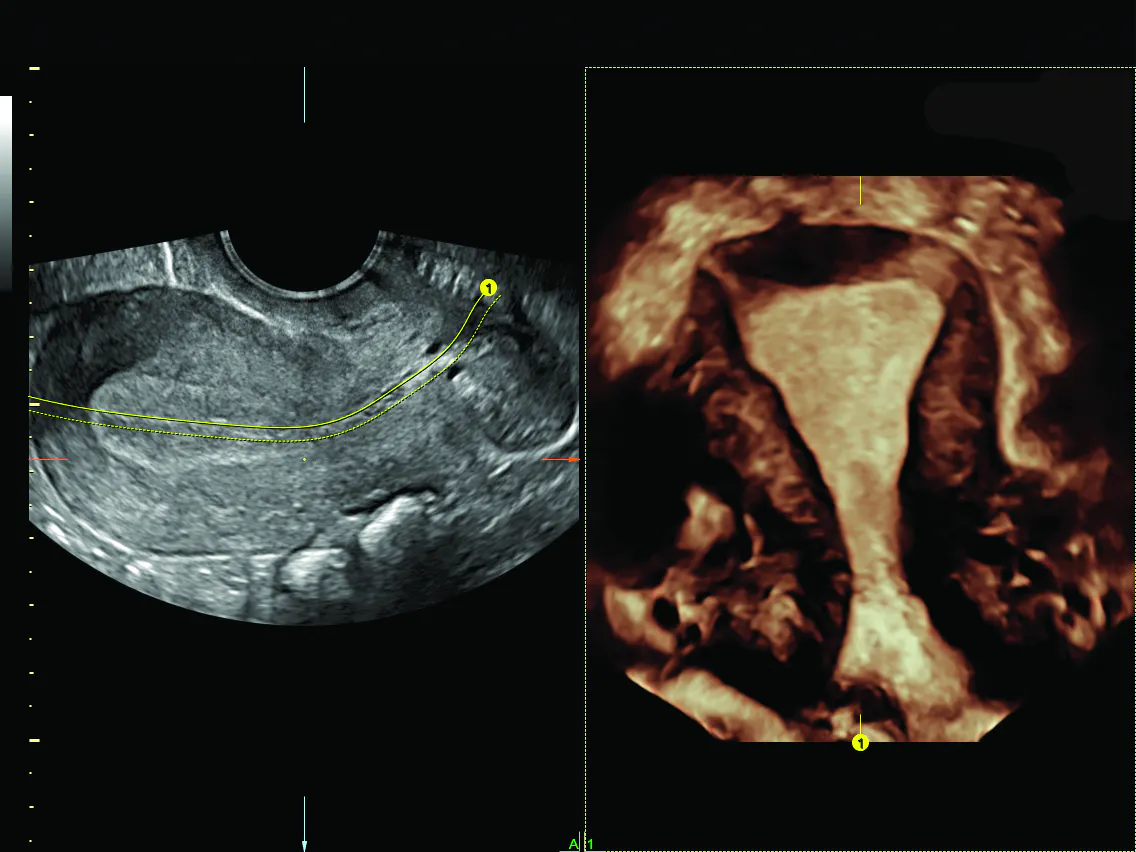
Coronal endometrium with OmniView; transvaginal ultrasound infertility image.
The real advantage of performing an ultrasound when screening for infertility symptoms is that it provides a multitude of information besides the antral follicle count, including the structural anatomy of the pelvic organs. The presence of other gynecologic pathology that might impact fertility, such as submucous fibroids, endometrial polyps, endometriomas and hydrosalpinx, can also be identified at the time of the pelvic ultrasound. It can evaluate each ovary individually and gauge its location and accessibility should IVF become a consideration. A 3D pelvic ultrasound is particularly helpful when congenital anomalies are suspected. The coronal view provides superb visualization of the arcuate versus septate uterine cavity and the entire uterine configuration.
Ultimately, the patient chooses whether to pursue any fertility workup, abbreviated or extensive. Her chief complaint may not be life-threatening or even lead to a diagnosis, but it's important to address her concerns nonetheless. Focus on your patient's infertility symptoms and keep it simple with 3D ultrasound when trying to diagnose infertility.