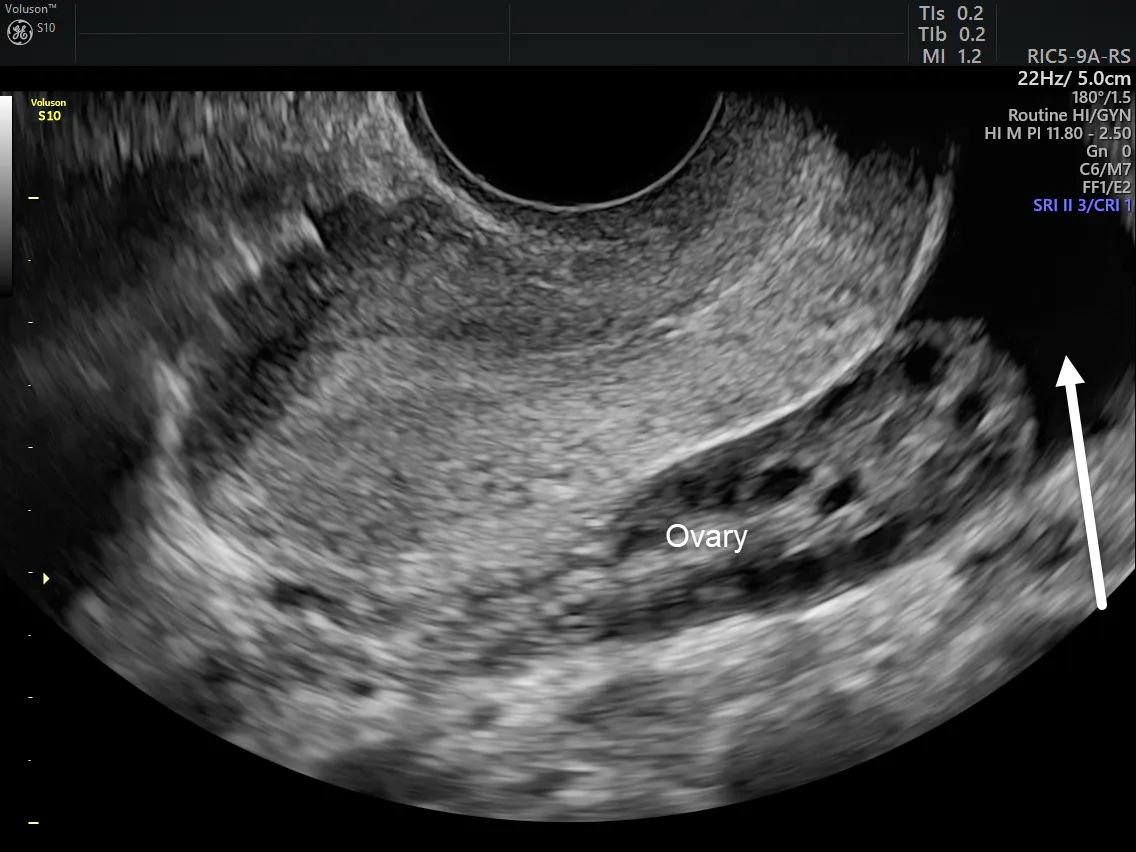
The female pelvis is a complex and ever-changing area of the human body, and the pouch of Douglas is a particular area of contrasts. Also known as the cul-de-sac, the pouch of Douglas exists between the uterus and the rectum, and it is the most dependent area of the pelvis, where fluids pool.
Physiologic and pathologic cul-de-sac fluid takes many forms. Menstrual blood that has refluxed through the fallopian tubes and fluids related to ovulation or ruptured cysts settle in it. Likewise, blood from a ruptured ectopic pregnancy, inflammatory debris from a pelvic or appendiceal infection and ascites due to malignancy, liver or cardiac failure may collect here. The amount may be copious or simply a small bit that is noted on routine ultrasound evaluation.
What Is the Pouch of Douglas?
The area in question is situated in close proximity to the posterior vaginal fornix, which provides a potential keyhole for access to the pelvic cavity. Diagnostic culdocentesis, drainage of cul-de-sac fluid collections and abscesses, and biopsies of pelvic cul-de-sac masses are examples of procedures that can be performed. Even minimally invasive actions, such as egg retrievals for IVF or bilateral tubal ligations, have been accomplished via this route. With the development and advancement of ultrasound technology, the assessment of the type and amount of fluid in the pouch of Douglas has improved our ability to categorize what's found there. At the same time, 3D ultrasound has thankfully reduced the number of invasive and often painful procedures performed via the posterior vaginal fornix.
This small, seemingly insignificant and shapeless space was named after an esteemed 18th-century Scottish physician and anatomist who lived in London and cared for women during childbirth. Dr. James Douglas was the queen's personal doctor. He also performed dissections in his home and published his findings and observations on a broad range of subjects. His surviving papers and anatomic drawings are preserved at the University of Glasgow and his immortality assured with several anatomic landmarks carrying his name, including the pouch of Douglas.
What to Look for in the Pouch of Douglas
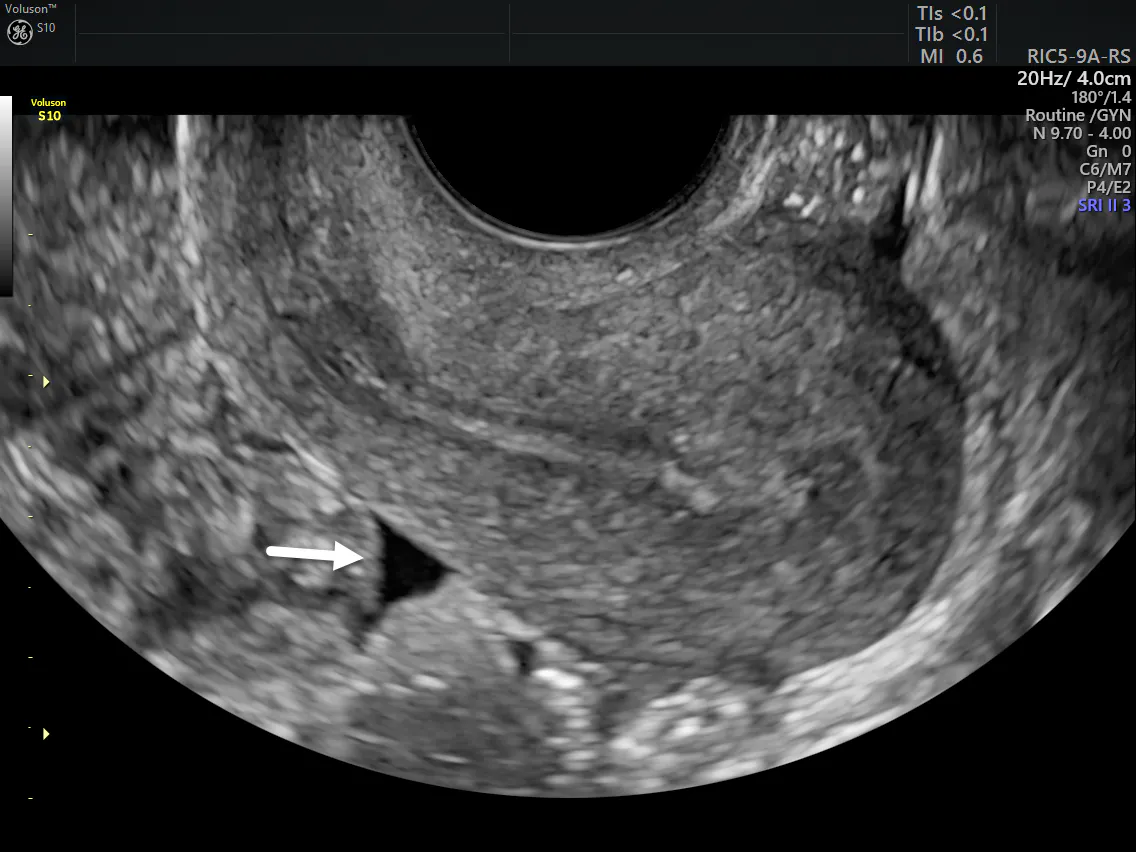
Studies published in 1982 in Radiology and in 1998 in the Journal of Ultrasound in Medicine demonstrated that echogenic masses and cul-de-sac fluid on transvaginal ultrasound are highly predictive of the finding of clotted blood and hemoperitoneum. Inflammatory effusions can have a variety of ultrasound features depending on the stage of the disease process. The discovery of filmy adhesions in the cul-de-sac fluid is suggestive of a past or chronic infection. A full urinary bladder may displace pelvic fluid out of the pouch of Douglas. This could lead to the mistaken diagnosis of ascites, which would have significant clinical implications.
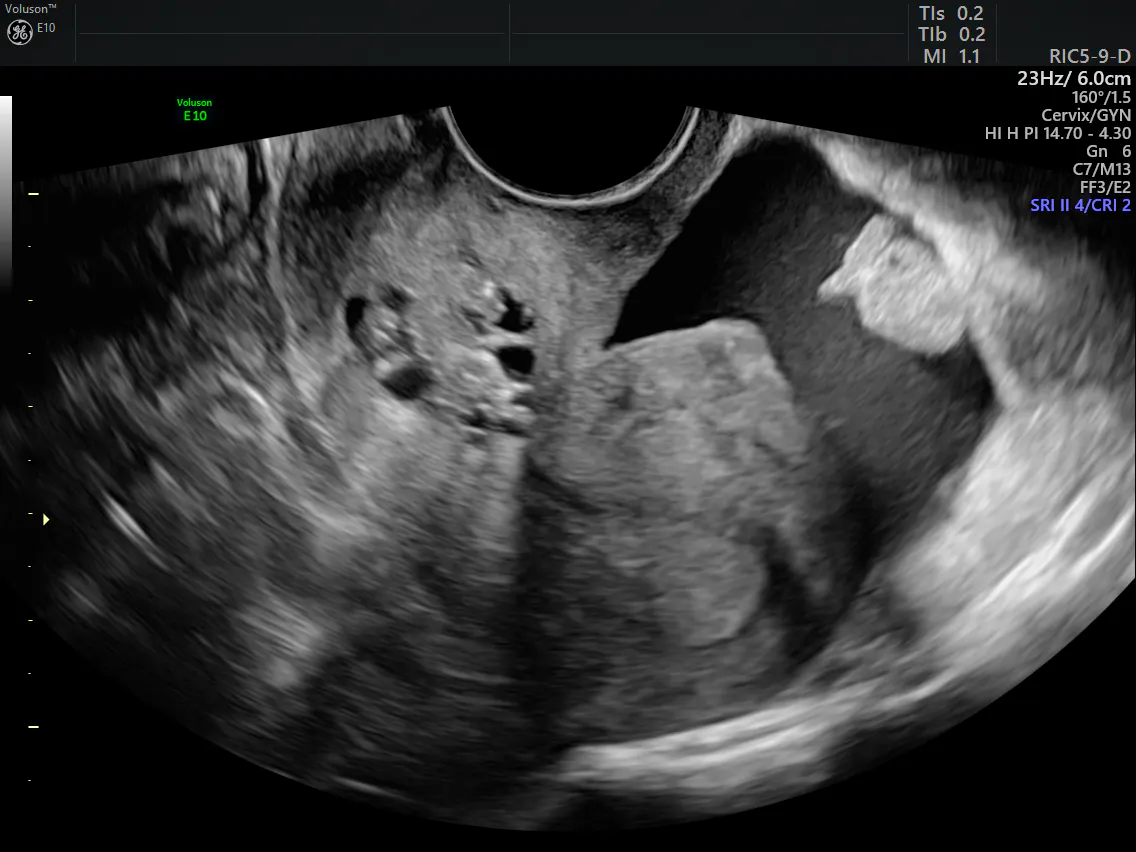
The ultrasound definition of ascites has been described as fluid filling the pouch of Douglas and extending beyond the fundus of the uterus. A better definition or actual quantification of the fluid is needed as the size of a uterus varies from individual to individual. In 2010, a study published in the journal Ultrasound in Obstetrics & Gynecology determined that patient height and weight did not appreciably affect the calculation of pelvic fluid volumes up to 1 liter. Measurements of the largest pocket of fluid were taken in three planes: height, length and depth. If the fluid surrounded the uterus and was found anterior and superior to the uterus as well, the volume of the uterus was calculated and subtracted from the measurement of the fluid pocket.
The study determined that the measurements of fluid volumes correlated with the amount of fluid instilled in the patient during the study and were reproducible. On the other hand, the absence of fluid in the pouch of Douglas may also have clinical significance. For example, in a patient with endometriosis, an obliterated cul-de-sac secondary to agglutination of the peritoneal surfaces from scarring caused by infiltrating endometriosis will prevent fluid from pooling here.
The pouch of Douglas should always be evaluated at the time of a transvaginal ultrasound, as the findings are often helpful in supporting a pelvic pain diagnosis. Because fluid from the pouch of Douglas protects the body from contamination, checking it on transvaginal ultrasound is vital.