A patient can expect a simple office procedure when they get their intrauterine device (IUD) removed. An experienced clinician will grasp the IUD strings with the polyp or ring forceps, ask the patient to take a deep breath or cough, and the IUD is easily removed with a gentle tug. However, if the IUD strings are not visible, the doctor should discuss the situation with their patient and offer an alternative method.
How to Remove an IUD
Here is a step-by-step protocol that doctors can follow for IUD removal:
- The endocervical canal is swept with a cervical cytology brush to identify the IUD strings in the endocervix and deliver them to where they can be grasped.
- If this fails, the endocervical canal is explored with alligator or Kelly forceps to identify and grasp the strings.
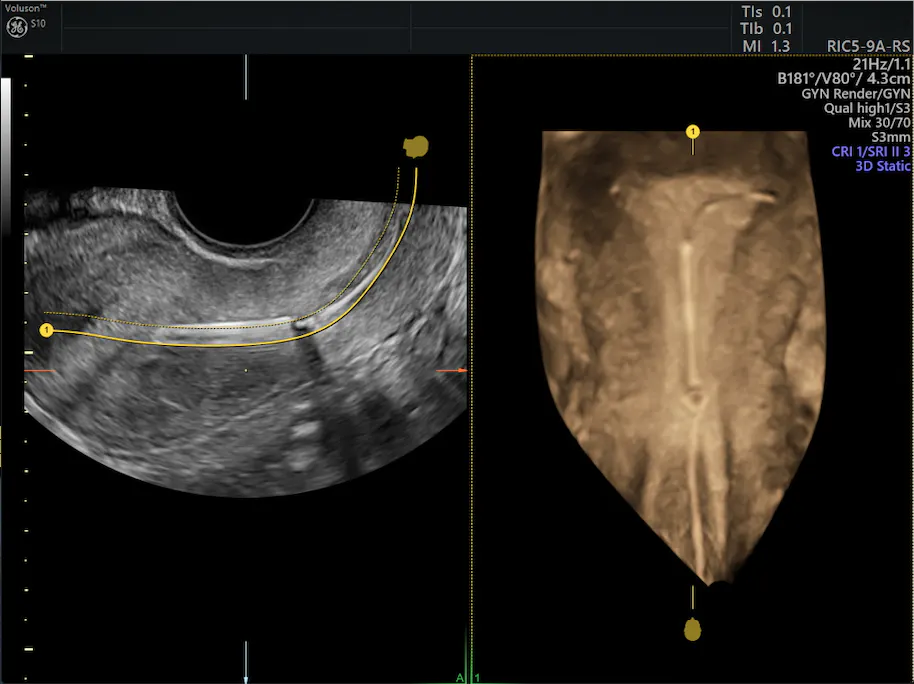
- If exploring the endocervical canal fails, an ultrasound can be performed to confirm the IUD is intrauterine. A 3D ultrasound is ideal if there is concern that an IUD arm is embedded, but standard 2D sagittal and transverse views will be adequate in identifying an intracavitary IUD.
- If the ultrasound confirms the presence of an intrauterine IUD, exploration of the uterine cavity is the next step. Some patients can tolerate this without analgesia, but others may need the cervix prepped with misoprostol, a paracervical block and/or intrauterine lidocaine installation.
- After obtaining consent, an IUD hook is introduced and advanced while rotating it in a clockwise fashion, thus attempting to ensnare the strings and remove the IUD. The clockwise rotation is continued as the hook is carefully withdrawn.
- Ultrasound guidance during office intrauterine exploration helps improve outcomes and is significantly more cost-effective when compared to removal in an operating room. It does require two people: One performs the IUD removal while the other conducts the transabdominal ultrasound in real time.
- If this fails to retrieve the IUD, the next step is office hysteroscopic removal of the IUD. An article in The Journal of Minimally Invasive Gynecology concludes this is successful in 97.4 percent of cases. Hysteroscopic removal requires specialized training, instrumentation and set-up.
A Few Words About Imaging IUDs
Patience and experience can help a clinician improve their imaging technique. The appearance of commonly used IUDs on ultrasound differs slightly.
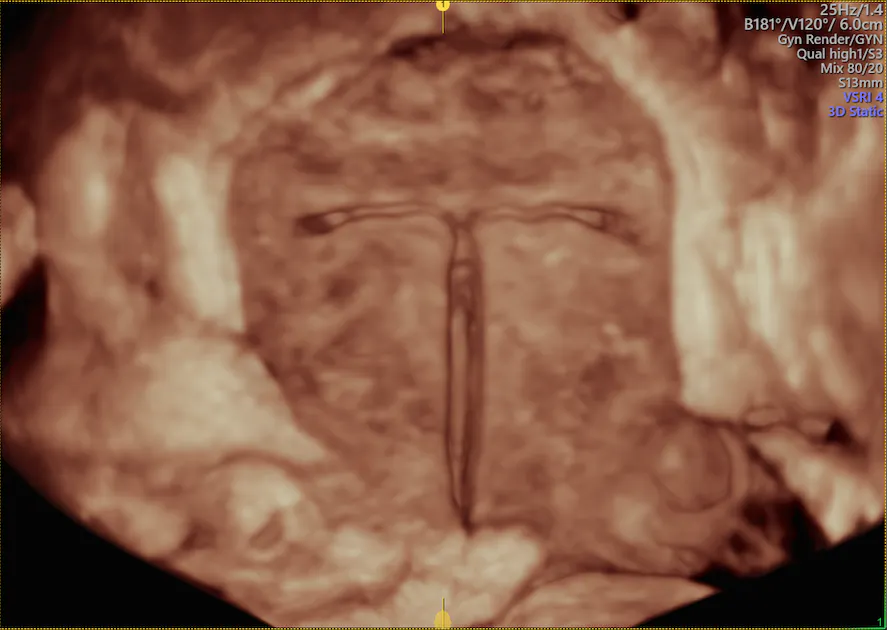
The levonorgestrel-releasing intrauterine system's plastic sleeve containing the progesterone casts an acoustic shadow that gives the appearance of two parallel lines. In addition, the highly echogenic strings can often be seen.
3D image of normal intrauterine device placement including string
3D image of normal IUD placement including string
- The copper IUD coils on the stem create a uniform echogenic appearance.
Copper IUD in normal placement alongside a uterine fibroid
- The Lippes Loop will show five intermittent echogenic shadows in 2D imaging, but in 3D, you can easily see the shape of the loop.
3D ultrasound image of Lippes Loop IUD
Partially expelled, rotated or embedded IUDs typically cause symptoms in patients. When this occurs, common complaints include pelvic pain, dyspareunia and irregular bleeding.
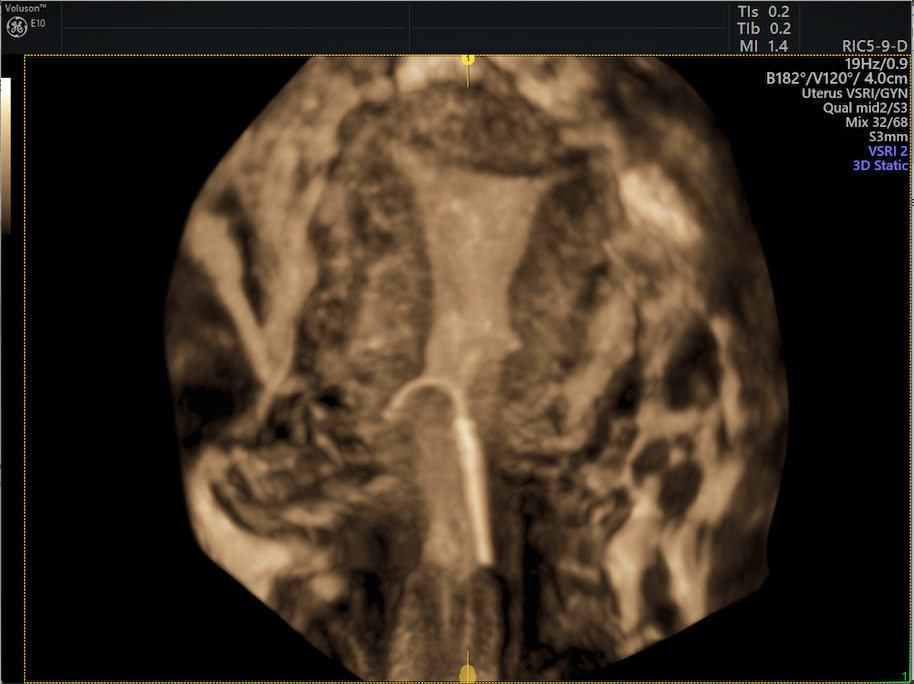
Partially expelled IUD needing IUD removal.
Partially expelled IUD
When a patient displays these symptoms, an ultrasound can be performed prior to attempted IUD removal in order to rule out a malpositioned IUD. If there is concern that the IUD has migrated through the myometrium and pierced the uterine serosa, additional imaging and laparoscopy is recommended. On the other hand, if the ultrasound confirms the IUD is in the uterine cavity, the above strategy would be advised.
IUDs provide significant reproductive benefits, but lost strings and migration are well-established risks of using them. When no identifiable strings are located during an exam, IUD removal can be completed successfully in the office with a few simple instruments under ultrasound guidance.