
Answering Advanced Maternal Age Pregnancy Questions with Ultrasound
Q&A with Dr. Ralf Menkhaus

Fertility declines with age, but with ultrasound, you can find out if a woman's biological clock is the barrier, & what can be done with reproductive tech.

It’s no secret that fertility declines with age. You know it. Most patients know it. But nobody wants to hear it when they’re struggling to get pregnant. It’s up to you to find out if her biological clock is the main barrier—and if she can find hope with assisted reproductive technology.
Ralf Menkhaus, M.D., of the Center for Fertility Treatment and Prenatal Diagnosis Minden in Germany, talks technology and highlights the ultrasound features that help him make faster, more confident clinical decisions in reproductive medicine.
Q: Many of your patients are over 35, and are coming to you for help because they can’t get pregnant. How important is ultrasound in evaluating these patients?A:Ultrasound is at the beginning of everything. Each one of my fertility patients has a 3D scan of the uterine cavity to see if there’s an anatomical reason—like a myoma or a septate uterus—why she can’t get pregnant. Ultrasound also helps me assess the ovarian reserve. Counting antral follicles in a 3D volume of the ovary is more exact than counting with 2D—and it’s more patient friendly. A volume can be taken quickly, and the counting can be done offline without the patient in the office.
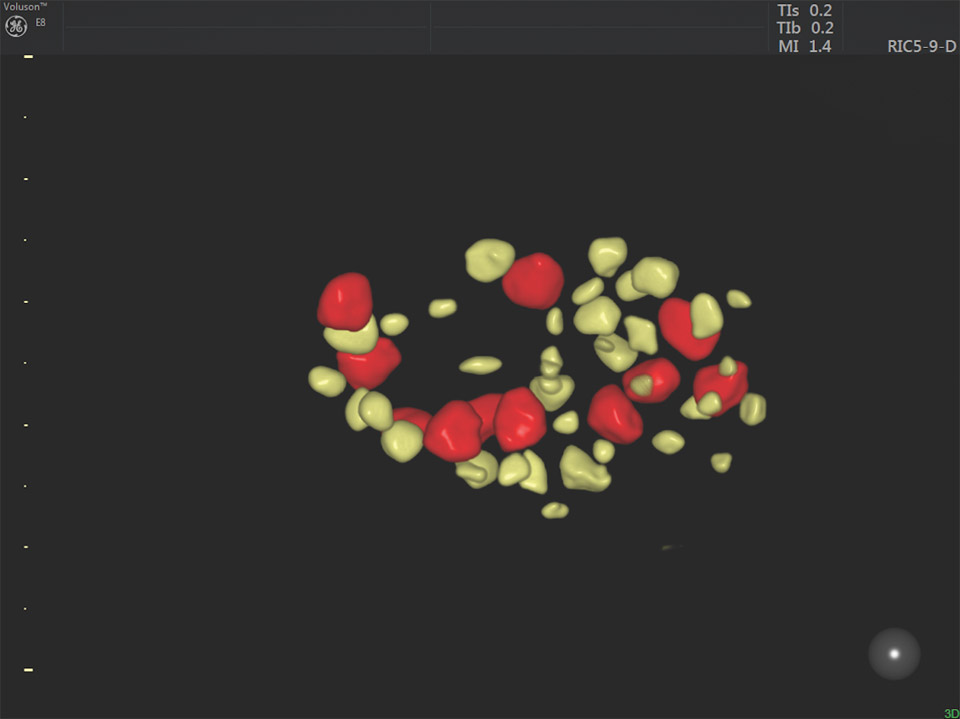
3D volume of ovary with SonoAVCantral to evaluate ovarian reserve
Q: What is the advantage of ultrasound over hysteroscopy and laparoscopy—two procedures still utilized by many physicians to assess fertility in patients?
A:Ultrasound is the first choice to assess the uterus and the ovaries. The possibility of 3D reconstruction of the uterine cavity makes hysteroscopy partially redundant. Ultrasound is also much quicker and it doesn’t harm the patient. It isn’t painful and it’s more cost-effective. It is the same with tubal patency. Although laparoscopy is still the so-called “gold standard,” we will just do a sonohysterography, and in most cases that will be sufficient.
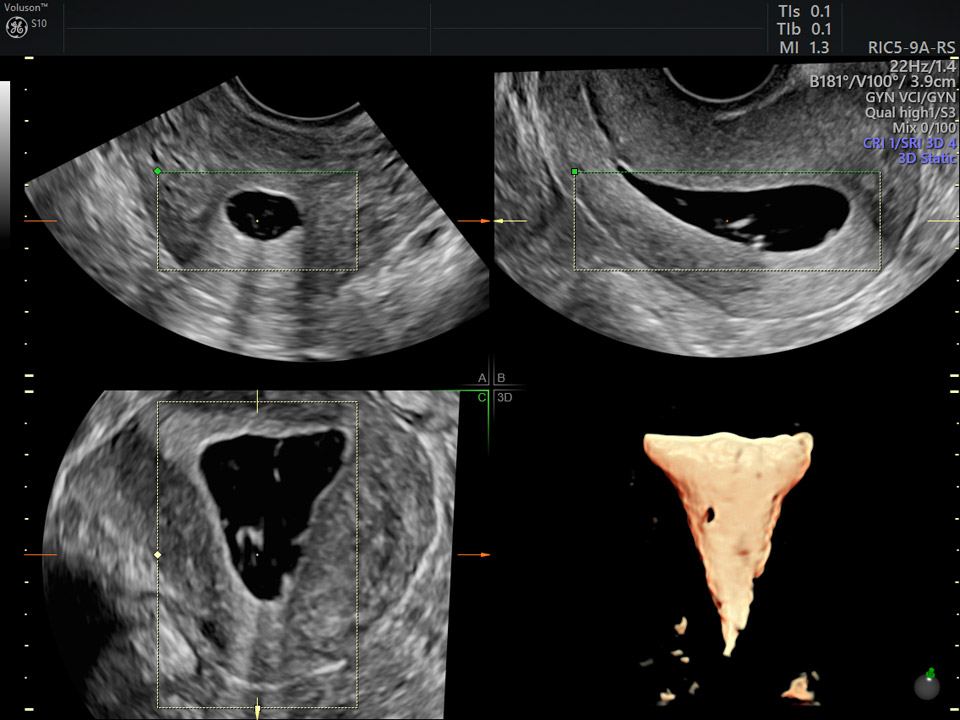
3D ultrasound Saline Infused Sonohysterogram
Q: What ultrasound technology do you use in your practice and how is it helpful in accessing fertility patients?
A:We use Volsuon™ and I believe they are the best machines and help us make the best diagnoses. The resolution is great—even in obese patients. I use many of the different features in my daily practice. I can look at any plane from a 3D volume using OmniView. It allows me to see irregularly shaped structures that can’t be seen in 2D. Another feature, Volume Contrast Imaging (VCI) provides better tissue differentiation so I can get a really good look at the uterine cavity.
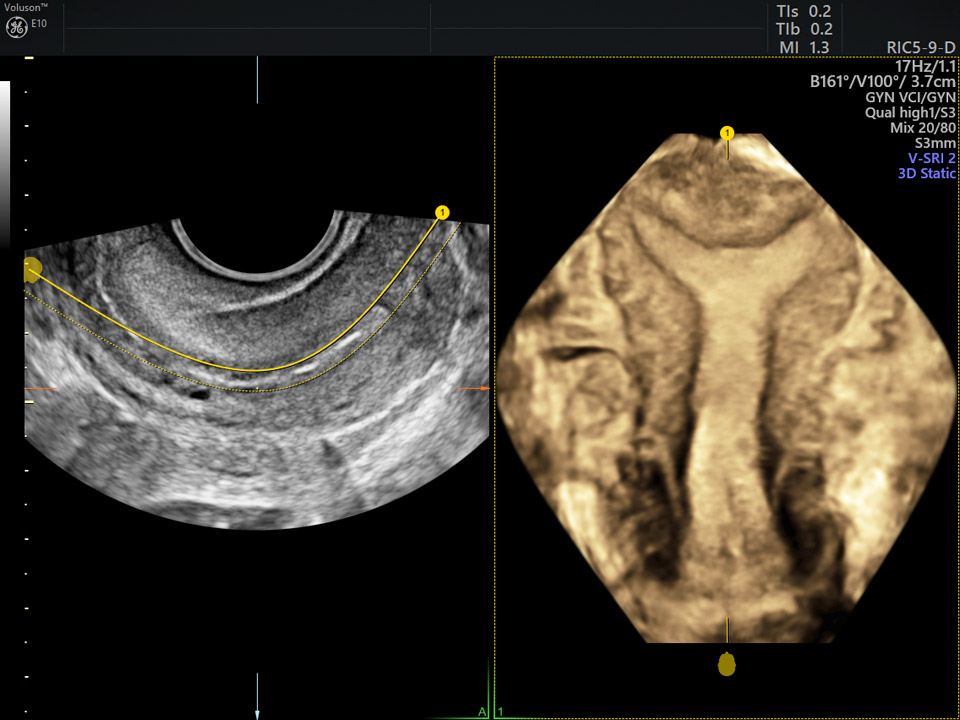
3D Advanced VCI with OmniView of normal uterine cavity
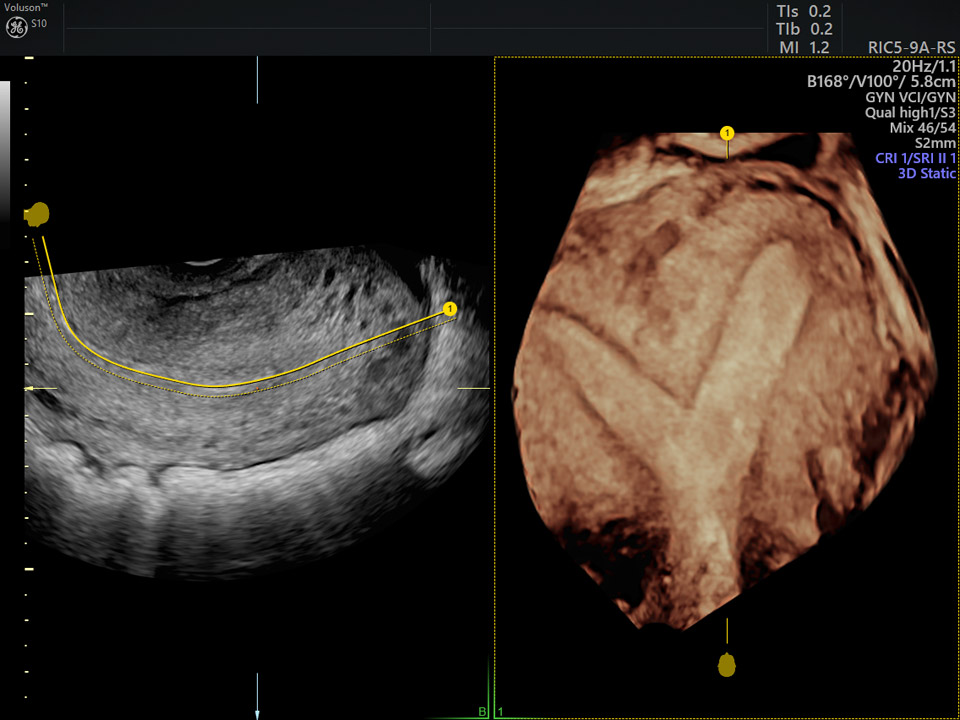
3D OmniView of subseptate uterus
Q: How does Voluson’s SonoAVC™ feature play a role in both evaluating patients who are struggling with infertility and those undergoing IVF treatment?
A:We use SonoAVC™antral to count the small follicles < 10mm to assess ovarian reserve. We take the volume of the whole ovary and then the calculation is automatic. SonoAVC™follicle is necessary to monitor a stimulation cycle. Using volume and automated 3D counting of all follicles is more exact than measuring only the biggest follicles with 2D, using only two planes. Utilizing SonoAVC™follicle is the most exact way to know when to induce ovulation because I want mature oocytes for the best possible outcome.
Q: What is the value of technology in your practice?A:Having new technology is important to me. I feel more confident, especially in malformation scans. I want things to be as exact as possible—and that depends a lot on image quality. I can really tell a difference between the new and old machines. The image quality has improved so much over the last several years. It’s incomparable. I also think it makes sense to buy high-tech equipment like Voluson because it’s good for your reputation. Patients will hear about the technology or even take note during an exam that it’s the best ultrasound equipment and want to see you.
-
What causes infertility?
-
A Voluson 3D transvaginal ultrasound offers real advantages when screening for infertility symptoms. Learn how Dr. Hanson manages fertility testing and sign up to Stay Informed. Understanding infertility symptoms before the disease.
-
Using pelvic ultrasound to screen the female reproductive organs for structural causes of infertility is one of the best first steps when beginning an infertility assessment. Voluson 2D and 3D ultrasound is used to assess uterine shape, size and provides views that allow you to assess for normal anatomy or pathology. Learn more about how Voluson can help enhance communication with your patients. What is infertility? What patients want to know.
-
Learn more about how Voluson ultrasound systems continually push the boundaries of Reproductive Medicine imaging to give you simple, yet innovative tools to help you and your patients achieve their dream of a successful pregnancy
-
Learn more from Dr. Angela Palumbo about how Voluson’s SonoAVC™ technology can benefit your Assisted Reproductive Medicine practice.
-
It’s simple math: the higher number of quality eggs a woman has, the greater her chances of having a baby. That’s why accurate follicular measurements during stimulation are critical in the IVF process. These calculations dictate timing—and missed follicles could mean missed opportunities. Learn more from Dr. Angela Palumbo.
-
Reproductive Medicine & IVF. Learn more about the past, present and future of IVF and reproductive medicine, and find the latest information that can help patients on their fertility journeys.
-
By catering to the concerns of women of fertility age, gynecologists can develop strong relationships that can last well past menopause.
-
Reproductive aging in women has an ovarian and uterine component. Doctors should use ultrasound and blood tests to assess ovarian reserve and oocyte health.
-
When trying to identify symptoms of infertility in women, transvaginal ultrasound should be the first test gynecologists recommend in diagnosing infertility.
-
Female Infertility Workup: Explaining Everything from Hormone Levels to Laparoscopy. From low-cost, non-invasive ultrasounds to laparoscopic surgery, reproductive endocrinologists now have many tools to include in a female infertility workup.
-
What You Should Know About Congenital Uterine Anomalies. 3D ultrasound enables physicians to diagnose possible congenital uterine anomalies in women with infertility or repeat adverse pregnancy outcomes.
-
What to Know About The Causes of Infertility, Evaluation and Treatment. Many patients have questions and concerns about diagnoses, treatments, and causes of infertility.
-
Learn more from Fiona Schwab, GE Healthcare’s Clinical Lead for Reproductive Medicine, about how ultrasound innovation tools can help turn your patient’s dream of a successful pregnancy into a reality.
-
Try out this fun exercise and learn more about the benefits of ultrasound in GYN diagnosis.


